Homeostasis Module
Water Balance and Electrolytes
Learning Objectives
By the end of this section, you will be able to:
- Explain the importance of water in the body
- Contrast the composition of the intracellular fluid with that of the extracellular fluid
- Correctly use medical terminology to describe abnormal electrolyte concentrations
- Explain how water balance is maintained, focusing on the role of the hypothalamus, the kidneys, and anti-diuretic hormone
- Describe the causes and consequences of water imbalance
The chemical reactions of life take place in aqueous solutions. The dissolved substances in a solution are called solutes. In the human body, solutes vary in different parts of the body, but may include proteins—including those that transport lipids, carbohydrates, and, very importantly, electrolytes. Often in medicine, a mineral dissociated from a salt that carries an electrical charge (an ion) is called and electrolyte. For instance, sodium ions (Na+) and chloride ions (Cl–) are often referred to as electrolytes.
In the body, water moves through semi-permeable membranes of cells and from one compartment of the body to another by a process called osmosis. Osmosis is basically the diffusion of water from regions of higher concentration to regions of lower concentration, along an osmotic gradient across a semi-permeable membrane. As a result, water will move into and out of cells and tissues, depending on the relative concentrations of the water and solutes found there. An appropriate balance of solutes inside and outside of cells must be maintained to ensure normal function.
Body Water Content
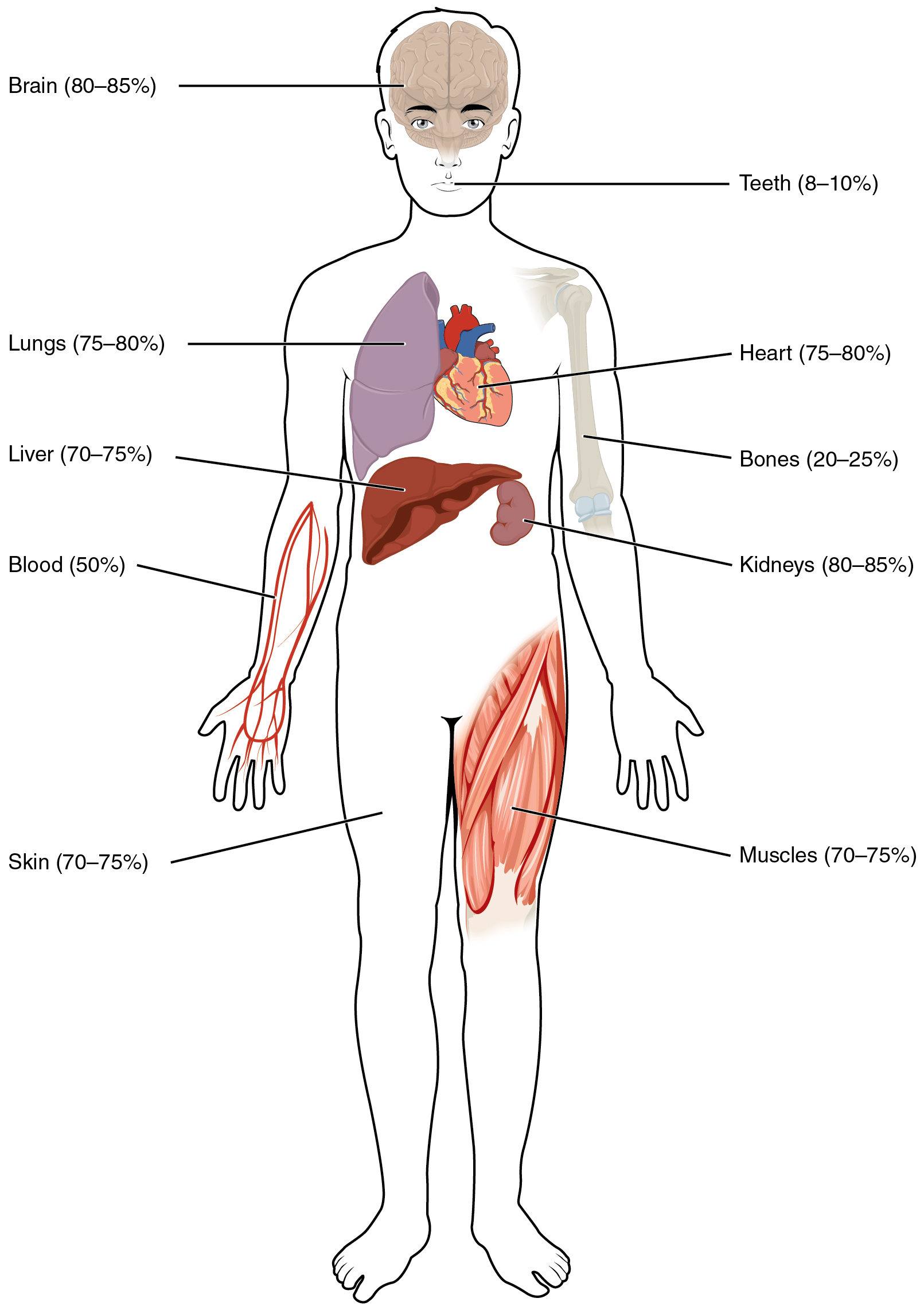
Human beings are mostly water, ranging from about 75 percent of body mass in infants to about 50–60 percent in adult men and women, to as low as 45 percent in old age. The percent of body water changes with development, because the proportions of the body given over to each organ and to muscles, fat, bone, and other tissues change from infancy to adulthood (Figure 1). Your brain and kidneys have the highest proportions of water, which composes 80–85 percent of their masses. In contrast, teeth have the lowest proportion of water, at 8–10 percent.
Fluid Compartments
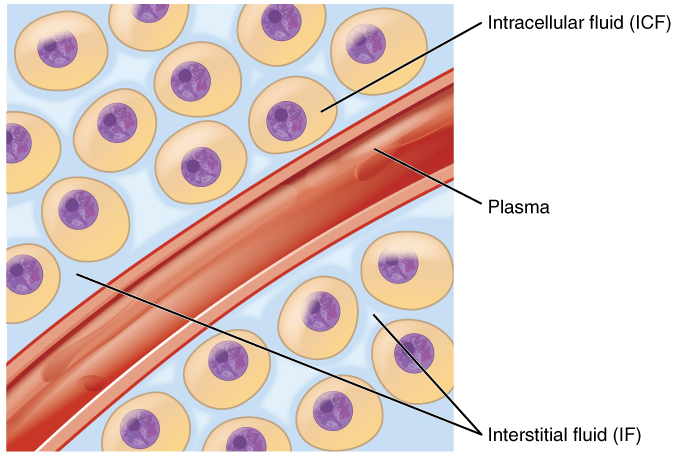
Body fluids can be discussed in terms of their specific fluid compartment, a location that is largely separate from another compartment by some form of a physical barrier. The intracellular fluid (ICF) compartment is the system that includes all fluid enclosed in cells by their plasma membranes. Extracellular fluid (ECF) surrounds all cells in the body. Extracellular fluid has two primary constituents: the fluid component of the blood (called plasma) and the interstitial fluid (IF) that surrounds all cells not in the blood (Figure 2).
Intracellular Fluid (ICF)
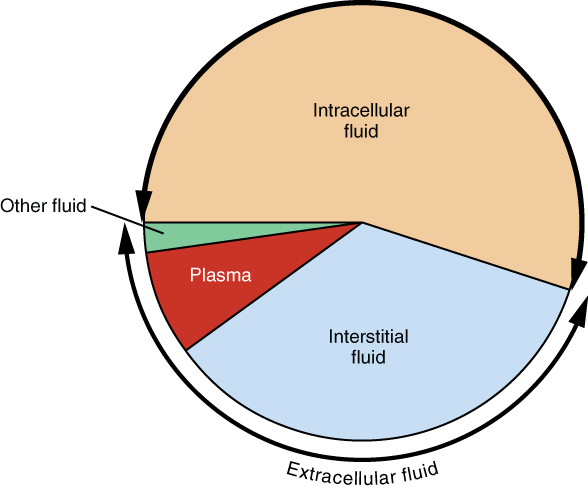
The ICF lies within cells and is the principal component of the cytosol/cytoplasm. The ICF makes up about 60 percent of the total water in the human body (Figure 3). This fluid volume tends to be very stable, because the amount of water in living cells is closely regulated.
Extracellular Fluid (ECF)
The ECF accounts for the other one-third of the body’s water content. Approximately 20 percent of the ECF is found in plasma. Plasma travels through the body in blood vessels and transports a range of materials, including blood cells, proteins (including clotting factors and antibodies), electrolytes, nutrients, gases, and wastes. Gases, nutrients, and waste materials travel between capillaries and cells through the interstitial fluid (IF). Cells are separated from the IF by a selectively permeable cell membrane that helps regulate the passage of materials between the IF and the interior of the cell.
Composition of Body Fluids
The compositions of the two components of the ECF—plasma and IF—are more similar to each other than either is to the ICF (Figure 4). Blood plasma has high concentrations of sodium, chloride, bicarbonate, and protein. The IF has high concentrations of sodium, chloride, and bicarbonate, but a relatively lower concentration of protein. In contrast, the ICF has elevated amounts of potassium, phosphate, magnesium, and protein. Overall, the ICF contains high concentrations of potassium and phosphate (HPO42−HPO42−), whereas both plasma and the ECF contain high concentrations of sodium and chloride.
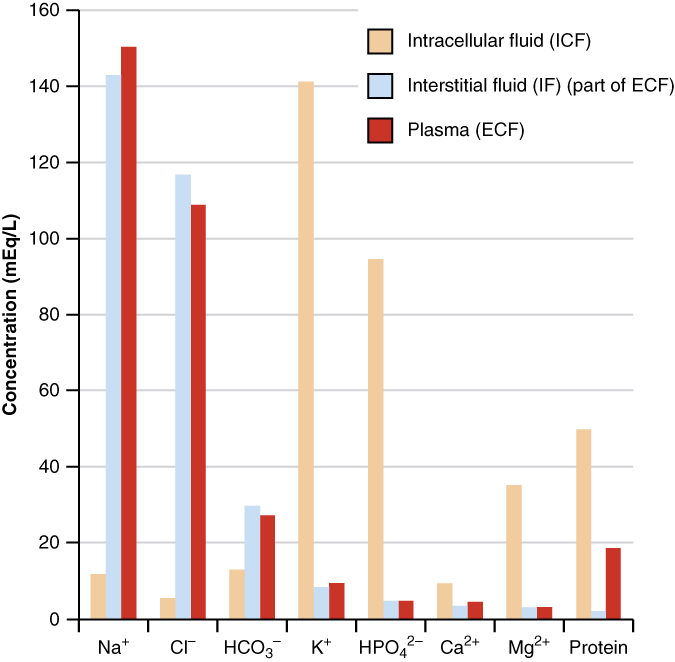
The ions in plasma also contribute to the osmotic balance that controls the movement of water between cells and their environment. Imbalances of these ions can result in various problems in the body. Adjustments in respiratory and renal functions allow the body to regulate the levels of these ions in the ECF.
Water Balance
On a typical day, the average adult will take in about 2500 mL of aqueous fluids. Although most of the intake comes through the digestive tract, about 300 mL per day is generated metabolically, in the last steps of aerobic respiration. Additionally, each day about the same volume (2500 mL) of water leaves the body by different routes; most of this lost water is removed as urine. The kidneys also can adjust blood volume though mechanisms that draw water out of the filtrate and urine. Some water is lost through sweat and stool. Water is also lost through the skin through evaporation from the skin surface without overt sweating and from air expelled from the lungs. This type of water loss is called insensible water loss because a person is usually unaware of it.
Regulation of Water Content
Osmolality is the ratio of solutes in a solution to a volume of solvent in a solution. Plasma osmolality is thus the ratio of solutes to water in blood plasma. A person’s plasma osmolality value reflects his or her state of hydration. A healthy body maintains plasma osmolality within a narrow range, by employing several mechanisms that regulate both water intake and output.
Drinking water is considered voluntary. So how is water intake regulated by the body? Consider someone who is experiencing dehydration, a net loss of water that results in insufficient water in blood and other tissues. The water that leaves the body, as exhaled air, sweat, or urine, is ultimately extracted from blood plasma. As the blood becomes more concentrated, the thirst response—a sequence of physiological processes—is triggered (Figure 5).
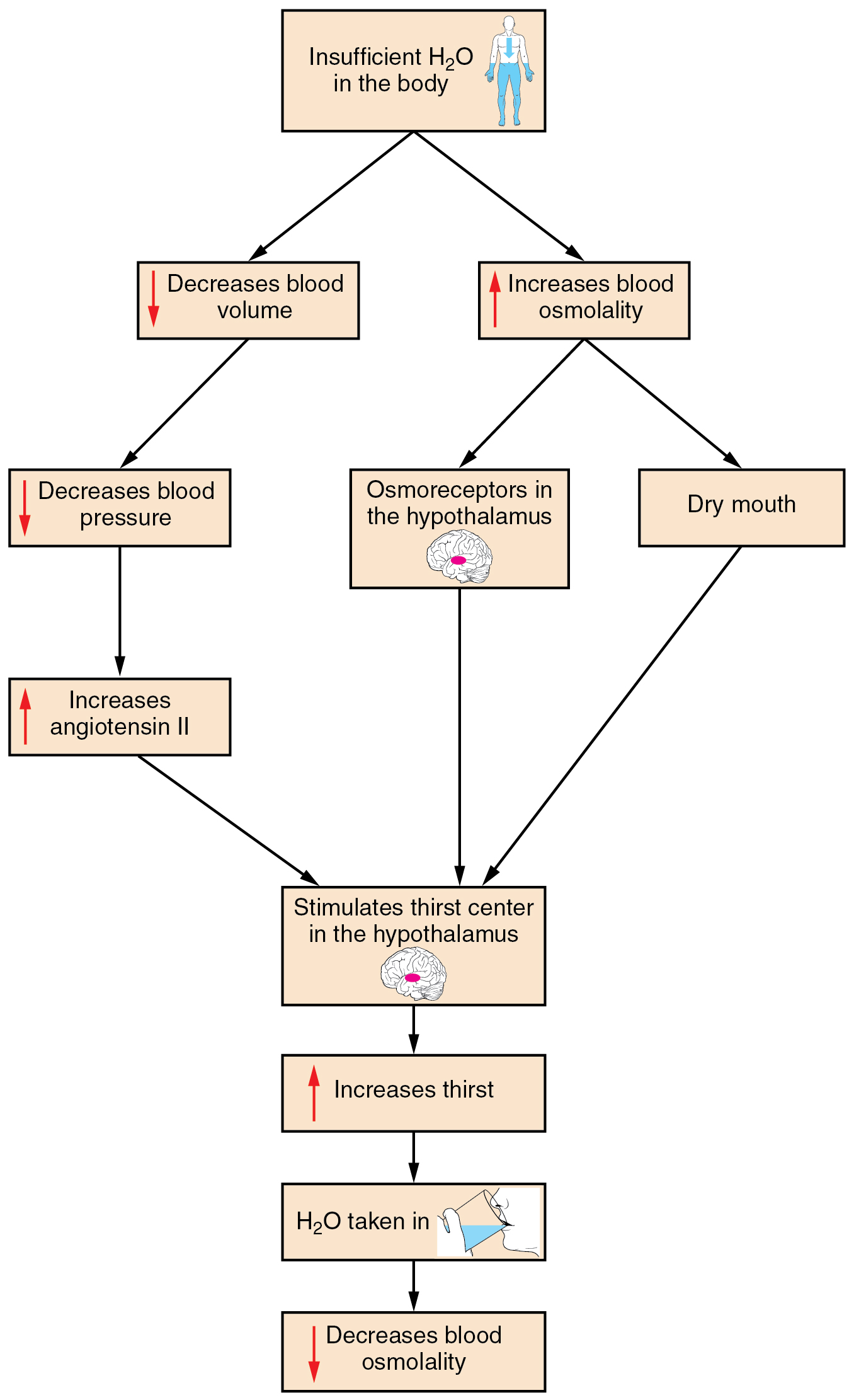
Osmoreceptors are sensory receptors in the thirst center in the hypothalamus that monitor the concentration of solutes (osmolality) of the blood. If blood osmolality increases above its ideal value, the hypothalamus transmits signals that result in a conscious awareness of thirst. To conserve water, the hypothalamus of a dehydrated person also sends signals via the sympathetic nervous system to the salivary glands in the mouth. The signals result in a decrease in watery, serous output (and an increase in stickier, thicker mucus output). These changes in secretions result in a “dry mouth” and the sensation of thirst.
The hypothalamus of a dehydrated person also releases antidiuretic hormone (ADH) through the posterior pituitary gland (Figure 7).
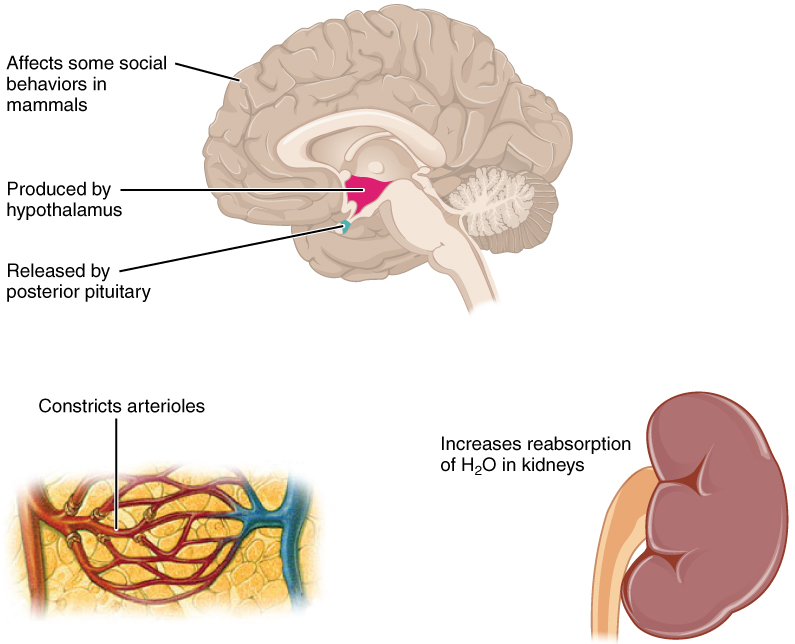
ADH constricts the arterioles in the peripheral circulation, which reduces the flow of blood to the extremities and thereby increases the blood supply to the core of the body. ADH also increases the water permeability of the renal collecting tubules to move water from the urine through the walls of the collecting tubules, leading to more reabsorption of water into the bloodstream.
Decreased blood volume resulting from water loss also impacts the kidney’s renin-angiotensin hormonal system (Figure 6). It increases the production of the active form of the hormone angiotensin II, which helps stimulate thirst, but also stimulates the release of the hormone aldosterone from the adrenal glands. Aldosterone increases the reabsorption of sodium and excetion of potassium in the distal tubules of the nephrons in the kidneys, and water follows this reabsorbed sodium back into the blood.
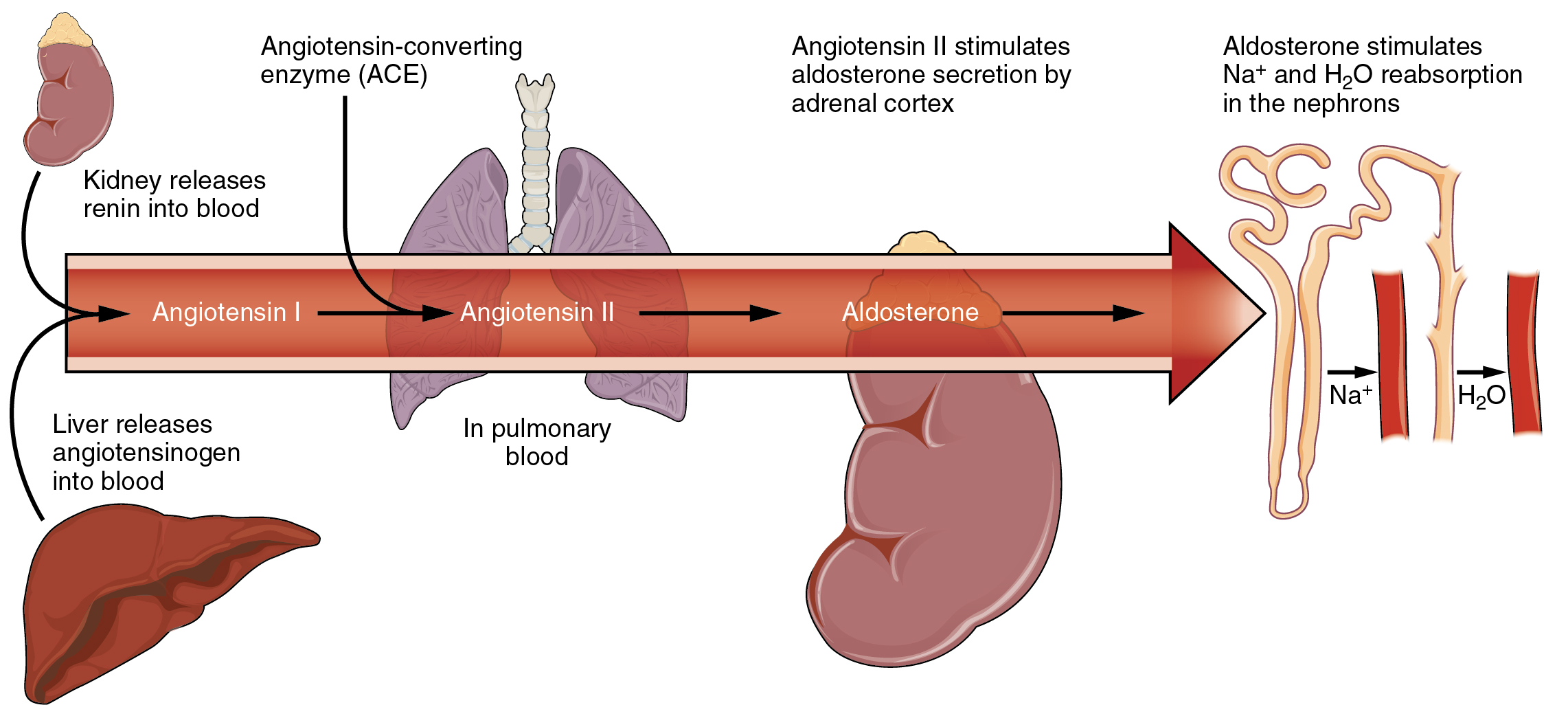
Water Imbalance
If adequate fluids are not consumed, dehydration results and a person’s body contains too little water to function correctly. A person who repeatedly vomits, who has diarrhea may become dehydrated, or who with burn wound exudates, can become dangerously dehydrated very quickly. Endurance athletes such as distance runners often become dehydrated during long races with increased sweating. Dehydration can be a medical emergency, and a dehydrated person may lose consciousness, become comatose, or die, if his or her body is not rehydrated quickly.
If a person’s body contains too much water, through either excess intake or inadequate output, water intoxication can occur. Excess body water content may be observed in a person who drinks too much water (e.g., polydipsia) or those with a failure in water regulatory mechanisms (e.g., kidney failure). Water intoxication can also be a result of medical errors, such as IV fluid overload. The first observable symptoms of water intoxication includes headaches, confusion, changes in behaviour, and drowsiness. Water intoxication can lead to vomitting, nausea, muscle weakness, bradycardia, cerebral edema, seizures, coma or death.
Go Further
- A Video on Fluids and Electrolytes by Dr. John Campbell.

