Central Nervous System Regulation, Mood, and Cognition
8.8 Antimania
Open Resources for Nursing (Open RN)
Mood stabilizers are used to treat bipolar affective disorder. Lithium was the first medication used to treat this disorder and is sometimes referred to as an anti-mania drug because it can help control the mania that occurs in bipolar disorder. Lithium must be closely monitored with a narrow therapeutic range.[1]
Lithium
Mechanism of Action
Lithium alters sodium transport in nerve and muscle cells and causes a shift toward intraneuronal metabolism of catecholamines, but the specific biochemical mechanism of lithium action in mania is unknown.[2]
Indications for Use
Lithium is indicated in the treatment of manic episodes of bipolar disorder and as a maintenance treatment for individuals with a diagnosis of bipolar disorder.
Nursing Considerations Across the Lifespan
Lithium must be closely monitored with a narrow therapeutic serum range of 0.6 to 1.2 mmol/L. [3] Serum sodium levels should also be monitored for potential hyponatremia.[4]
The drug is contraindicated in renal or cardiovascular disease, severe dehydration or sodium depletion, and to clients receiving diuretics because the risk of lithium toxicity is very high in such clients.
Lithium can cause fetal harm in pregnant women. Safety has not been established for children under 12 and is not recommended.
When given to a client experiencing a manic episode, lithium may produce a normalization of symptomatology within 1 to 3 weeks.[5]
Adverse/Side Effects
Black Box Warning: Lithium toxicity is closely related to serum lithium levels and can occur at doses close to therapeutic levels at 1.5 mEq/L. Facilities for prompt and accurate serum lithium determinations should be available before initiating therapy. Lithium can cause abnormal electrocardiographic (ECG) findings and risk of sudden death. Clients should be advised to seek immediate emergency assistance if they experience fainting, lightheadedness, abnormal heartbeats, or shortness of breath.
Signs of early lithium toxicity include diarrhea, vomiting, drowsiness, muscular weakness, and lack of coordination. At higher levels, giddiness, ataxia, blurred vision, tinnitus, and a large output of dilute urine may be seen. No specific antidote for lithium poisoning is known; treatment focuses on the elimination of the medication.
Fine hand tremor, polyuria, and mild thirst may also persist throughout treatment.[6],[7]
Client Teaching & Education
Clients should take medication as directed. It is important to note that antimanic drugs may increase dizziness and drowsiness. Additionally, if individuals have low sodium levels, it may predispose the client to toxicity. Clients should also be advised that weight gain may occur.
Now let’s take a closer look at the medication grid for lithium in Table 8.8.[8],[9]
Medication cards like this are intended to assist students to learn key points about each medication. Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication. Basic information related to each class of medication is outlined below. Prototype or generic medication examples are also hyperlinked to a free resource at Daily Med. On the home page, enter the drug name in the search bar to read more about the medication.
Table 8.7 Lithium Medication Card [10][11][12][13]
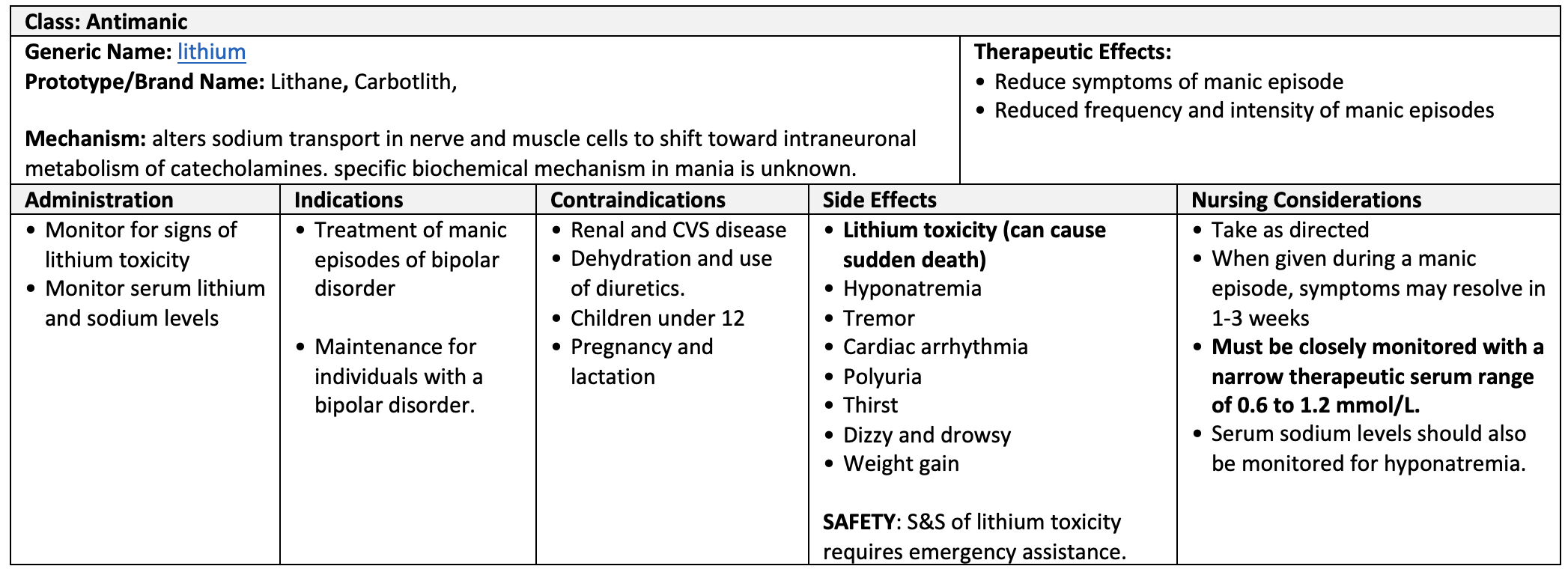
Clinical Reasoning and Decision-Making Activity 8.8
A 42-year-old male was recently diagnosed with bipolar disorder after his partner became concerned about his extreme highs and lows in moods. His high mood swings were often associated with grandiose ideas, gambling, risky sexual behavior, and shopping sprees that were causing the couple to go bankrupt. The physician prescribed lithium.
1. The client states, “The doctor told me I am having manic episodes. What does that mean?” What is the nurse’s best response?
2. The nurse knows that there is a risk of lithium toxicity. What are the symptoms of lithium toxicity, and how will it be prevented?
3. The client’s partner asks, “How quickly will the lithium work?” What is the nurse’s best response?
Note: Answers to the Critical Thinking activities can be found in the “Answer Key” sections at the end of the book.
Media Attributions
- lithium
- McCuistion, L., Vuljoin-DiMaggio, K., Winton, M, & Yeager, J. (2018). Pharmacology: A patient-centered nursing process approach. pp. 227-305. Elsevier. ↵
- This work is a derivative of Daily Med by U.S. National Library of Medicine in the public domain. ↵
- Medical Council of Canada. (2021). Clinical laboratory tests -Adult normal values. https://mcc.ca/objectives/normal-values/ ↵
- McCuistion, L., Vuljoin-DiMaggio, K., Winton, M, & Yeager, J. (2018). Pharmacology: A patient-centered nursing process approach. pp. 227-305. Elsevier. ↵
- This work is a derivative of Daily Med by U.S. National Library of Medicine in the public domain. ↵
- This work is a derivative of Daily Med by U.S. National Library of Medicine in the public domain. ↵
- McCuistion, L., Vuljoin-DiMaggio, K., Winton, M, & Yeager, J. (2018). Pharmacology: A patient-centered nursing process approach. pp. 227-305. Elsevier. ↵
- This work is a derivative of Daily Med by U.S. National Library of Medicine in the public domain. ↵
- McCuistion, L., Vuljoin-DiMaggio, K., Winton, M, & Yeager, J. (2018). Pharmacology: A patient-centered nursing process approach. pp. 227-305. Elsevier. ↵
- This work is a derivative of Daily Med by U.S. National Library of Medicine in the public domain. ↵
- RNPedia. (2021). https://www.rnpedia.com ↵
- OpenMD.Com at www.openmd.com ↵
- uCentral from Unbound Medicine. https://www.unboundmedicine.com/ucentral ↵
Cord-like bundle of axons located in the peripheral nervous system that transmits sensory input and response output to and from the central nervous system.

