Chapter 8: IV Therapy
8.3 Types of Venous Access
Critical Thinking Exercises: Questions, Answers, and Sources / References
- Differentiate different venous access devices: PVAD-short, midline catheter, peripherally inserted central catheter (PICC), percutaneous non hemodialysis central catheter, implanted venous access device (IVAD), and tunneled catheter. Provide one indication for each. Answer:
| Type of VAD | Characteristics |
| PVAD short | · PVAD-short sites are prone to phlebitis and infection in comparison to CVAD sites
· Easily monitored · can be inserted at the bedside. · CDC (2017) recommends that PVAD-shorts be replaced every 72 to 96 hours to prevent infection and phlebitis in adults. Other literature suggests that PVAD-short catheters be changed based on individual assessment of the site and not specific time frames (Gorski et al., 2012)
Indication: Used for infusions under six days and for solutions that are iso-osmotic or near iso-osmotic (CDC, 2017). |
| PVAD midline | · 5 to 20 cm long
· usually inserted into an antecubital fossa · catheter tip sits in the vein below the level of the axilla. · tip of the catheter sits in a vessel larger than a peripheral vein, it is significantly smaller than the superior vena cava (SVC). As such the types of drugs and solutions that can be safely administered through a midline catheter are the same as a PVAD-short (Rosenthal, 2007).
Indication: Used for IV therapy longer than a PVAD-short although the literature is inconsistent in terms of how long. The range is from 6 days to 8 weeks (RNAO, 2005 / 2008). |
| CVADs (generally speaking) | · Usually the tip of the catheter terminates in the superior vena cava just above the right atrium.
· Femorally inserted CVADs, the tip of the catheter should sit in the inferior vena cava. · Large vein = ability to deliver fluids and/or medications that can be overly irritating (high or low pH, high osmolality) to small peripheral veins long term IV therapy and / or high osmololity medications / solutions · ability to access multiple lumens and deliver multiple medications or solutions simultaneously even if they are incompatible with each other (Fraser Health Authority, 2014) · ability to deliver large volumes quickly · ability to maintain IV access over a prolonged period of time (Perry et al., 2018). · Some CVADs have technology associated with them that allows for monitoring of central venous pressure
Indication: long term IV therapy; IV therapy with high osmolality medications |
| CVAD – Peripherally inserted central catheter (PICC) | · tip is located in the SVC.
· inserted through the antecubital fossa or upper arm (basilic or cephalic vein) & threaded the full length until the tip reaches the SVC. · held in place with sutures or a manufactured securement device for as long as there is no evidence of complications.
Indication: long term IV therapy; IV therapy with high osmolality medications |
| Tunnelled central venous catheter
|
· long-term CVC ie. months – years
· catheter tip in SVC · Insertion is a surgical procedure, in which the catheter is tunnelled subcutaneously under the skin in the chest area before it enters the SVC. · low infection rate due to aDacron cuff, an antimicrobial cuff surrounding the catheter near the entry site, which is coated in antimicrobial solution and holds the catheter in place after two to three weeks of insertion.
Indication: long term IV therapy; IV therapy with high osmolality medications, dialysis |
| Implanted venous access device (IVAD)
· aka implanted central venous catheter (ICVC); aka port-a-cath
|
· considered permanent
· catheter tip in SVC · device may be placed in the chest, abdomen, or inner aspect of the forearms. For some this is preferred because of body image. For others this is preferred because the unit is concealed under the skin, so it is ideal for those who like to swim or use a hot tub. IVADs are accessed by specially trained personnel using a non-coring needle.
Indication: long term IV therapy; IV therapy with high osmolality medications |
| Percutaneuos central venous catheter (CVC)—non hemodialysis
|
· tip in SVC
· longevity = days → months · Can be inserted at the bedside by specially trained physician or nurse. · inserted directly through the skin. The internal or external jugular, subclavian, or femoral vein is used. · Most commonly used in critically ill patients. · Usually held in place with sutures or a manufactured securement device.
|
Sources:
Center for Disease Control (2017). Guidelines for the Prevention of Intravascular Catheter-Related Infections: Summary of Recommendations. https://www.cdc.gov/infectioncontrol/guidelines/bsi/recommendations.html
Fulcher, E. M., & Fraser, M. S. (2007). Introduction to intravenous therapy for health professionals. St Louis, MO: Elsevier.
Gorski, L., Hallock, D., Kuehn, S., Morris, P., Russell, J., Skala, L. (2012). INS Position Paper Recommendations for Frequency of Assessment of the Short Peripheral Catheter Site. https://e58f7f8fa122555ac87a-8a1d6df4618501341882ba7daeabdf40.ssl.cf2.rackcdn.com/ins_913b61c0470f3e329882c67480b6fb4f.pdf
Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
Registered Nurses of Ontario. (2005) Supplement 2008. Nursing Best Practice Guideline: Care and Maintenance to Reduce Vascular Access Complications. http://rnao.ca/sites/rnao-ca/files/Care_and_Maintenance_to_Reduce_Vascular_Access_Complications.pdf
Rosenthal, K. (2007). Bridging the I.V. access gap with midline catheters. Nursing made incredibly easy. pp.18-20. https://www.rch.org.au/uploadedFiles/Main/Content/anaes/bridging_the_IV_access_gap_with_midline_catheters.pdf
2. Identify a situation where having a multilumen CVC is desired.
Answer: when multiple meds / solutions have to be given simultaneously; when medications / solutions are incompatible a multilumen allows for concurrent administration
- What is the difference between a non tunneled percutaneous catheter and a tunnelled catheter?
Answer: tunnelled catheters run underneath the skin before entry into the central vein. This allows these catheters to remain in place for an extended period (ie. dialysis).
Sources:
Fulcher, E. M., & Fraser, M. S. (2007). Introduction to intravenous therapy for health professionals. St Louis, MO: Elsevier.
Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
2. Name 3 benefits of a central line .
Answer: longevity compared with PVAD short IV access; able to infuse large volumes quickly; able to infuse highly irritating (think pH & osmolarity) medications and solutions
Sources:
Fulcher, E. M., & Fraser, M. S. (2007). Introduction to intravenous therapy for health professionals. St Louis, MO: Elsevier.
Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
3. Name 3 risks associated with IV therapy via a central venous catheter.
Answer: sepsis is more likely with central lines because of proximity to central circulation; risk of fluid overload because of proximity to central circulation and size of vein being infused; occlusion from fibrin / medication build up in the lumen
Source:
Baskin, J. L., Pui, C. H., Reiss, U., Wilimas, J. A., Metzger, L. M., Ribeiro, R. C., & Howard, S. C. (2009). Management of occlusion and thrombosis associated with long-term indwelling central venous catheters. Lancet, 374(9684), 159. doi: 10.1016/S0140-6736(09)60220-8.
British Columbia Institute of Technology (BCIT). (2015a). CVC complications worksheet. In, NURS 3020. BCIT BSN program. Vancouver, BC: BCIT.
Earhart, A. (2013). Central lines: Recognizing, preventing, and troubleshooting complications. American Nurse Today, 8(11). https://www.americannursetoday.com/central-lines-recognizingpreventing-and-troubleshooting-complications/
Fraser Health Authority. (2014). Clinical practice guidelines: Intravenous therapy. http://physicians.fraserhealth.ca/media/2014%2005%2015%20IV%20Therapy%20CPG%20FINAL.pdf.
Fulcher, E. M., & Frazier, M. S. (2007). Introduction to intravenous therapy for health professionals. St. Louis, MO: Elsevier.
Interior Health. (2012). Parenteral practices manual. http://insidenet.interiorhealth.ca/Clinical/parenteralccr/Pages/Manual.aspx.
Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
Prabaharan, B., & Thomas, S. (2014). Spontaneous migration of central venous catheter tip following extubation. Saudi Journal of Anaesthesia, 8(1), 131–133. doi: 10.4103/1658-354X.125975.
- Differentiate if the following characteristics are different when comparing PVAD short and midline catheters. Answer True (yes) or False (no)
| Characteristic | Answer | |
| a. | Catheter length is different | True. Midline catheters are longer than PVAD short catheters |
| b. | Where they can be inserted is different | True. PVAD shorts can theoretically inserted into shorter veins. |
| c. | Longevity – one can be left in longer than the other. | True. PVAD shorts are suggested to remain in situ up to 96 hours. Midline catheters are suggested to remain in situ up to 8 weeks. |
| d. | Comfort – one is more comfortable than the other | Not necessarily. It’ll depend on the location, the integrity of the site, patient perception |
Source:
Registered Nurses’ Association of Ontario (RNAO). (2005) Nursing best practice guideline: Care and maintenance to reduce vascular access complications [Revised 2008 supplement]. http://rnao.ca/sites/rnao-ca/files/Care_and_Maintenance_to_Reduce_Vascular_Access_Complications.pdf.
Rosenthal, K. (2007). Bridging the I.V. access gap with midline catheters. Nursing Made Incredibly Easy, pp.18-20. https://www.rch.org.au/uploadedFiles/Main/Content/anaes/bridging_the_IV_access_gap_with_midline_catheters.pdf.
- Identify the venous access device in each of the photos
A. 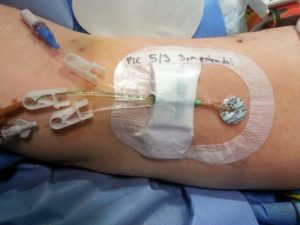 B.
B. 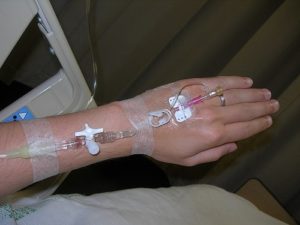 C.
C. 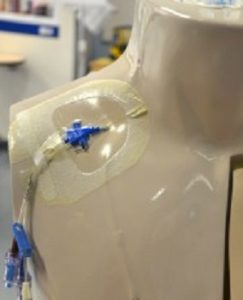
Answer: A = PICC ; B= PVAD short ; C = percutaneous non hemodialysis central line.
Attribution:
A. Omläggning av PICC [Conversion of PICC] by Nurseirie is used under a CC BY-SA 3.0 unported license.
B. Intravenous therapy is from Michaelberry at English Wikipedia and is used under a CC BY 3.0 Unported license.
C. Percutaneous non hemodialysis central line by author is licensed under a CC BY-SA 4.0 international license.
6. Match the correct venous access device with its appropriate description: PVAD short / CVAD / PICC
| Description | Type of VAD | |
| a. | Peripherally inserted venous access device that is relatively small in size | PVAD short |
| b. | Peripherally inserted central catheter often inserted into a vein in the upper arm | PICC |
| c. | The tip of the catheter is in a peripheral vein | PVAD short |
| d. | The tip of the catheter is in the superior vena cava | CVAD / PICC |
| e. | Carries risk of pulmonary edema when IV solutions are infused | PVAD short / CVAD / PICC |
| f. | Is a type of CVAD | PICC |
7. When a CVC is inserted into the femoral vein, where should the tip of the catheter be located?
a. femoral vein (incorrect)
b. inferior vena cava (correct)
c. iliac vein (incorrect)
d. renal vein (incorrect)
Source: Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
8. Pain and swelling in the patient’s chest wall, neck, and jaw on the side of PICC or central line insertion are potential signs and symptoms of
a. pinch-off syndrome (Incorrect)
b. vein or catheter thrombosis (Correct)
c. infusing irritating medications (Incorrect)
d. pneumothorax (Incorrect)
Source:
Earhart, A. (2013). Central lines: Recognizing, preventing, and troubleshooting complications. American Nurse Today, 8(11). https://www.americannursetoday.com/central-lines-recognizingpreventing-and-troubleshooting-complications/
9. Which statement correctly describes a fibrin layer on a PICC or Central line catheter?
a. It can form a flap on the catheter tip and act like a valve causing occlusion (Correct)
b. It develops when the tunica intima is damaged. (Incorrect)
c. It’s a thrombus extending from the vein wall to the catheter. (incorrect)
d. It occurs when platelets accumulate in a damaged area. (incorrect)
Sources:
Center for Disease Control (2017). Guidelines for the prevention of intravascular catheter-related infections: Summary of recommendations. https://www.cdc.gov/infectioncontrol/guidelines/bsi/recommendations.html.
Registered Nurses’ Association of Ontario (RNAO). (2005) Nursing best practice guideline: Care and maintenance to reduce vascular access complications [Revised 2008 supplement]. http://rnao.ca/sites/rnao-ca/files/Care_and_Maintenance_to_Reduce_Vascular_Access_Complications.pdf.
10. Which of the following medications would be used to dissolve clot / fibrin when a PICC line is suspected to be occluded?
a. alteplase (Correct)
b. contrast medium (Incorrect. Contrast medium is used for diagnostic purposes)
c. low-molecular-weight heparin (Incorrect. This is an anticoagulant and can’t dissolve clots)
d. unfractionated heparin (Incorrect. This is an anticoagulant and can’t dissolve clots)
Source: Registered Nurses’ Association of Ontario (RNAO). (2005) Nursing best practice guideline: Care and maintenance to reduce vascular access complications [Revised 2008 supplement]. http://rnao.ca/sites/rnao-ca/files/Care_and_Maintenance_to_Reduce_Vascular_Access_Complications.pdf.
11. Which of the following can be safely administered through a short peripheral I.V. catheter?
| a. | continuous vesicant chemotherapy | incorrect. This is highly irritating to the veins and would cause phlebitis. |
| b. | solutions with osmolarity greater than 500 mOsm/liter | incorrect. This is highly irritating to the veins and would cause phlebitis. |
| c. | parenteral nutrition containing more than 10% dextrose | incorrect. This solution has a high osmolalit, is highly irritating to the veins and would cause phlebitis to a peripheral vein. |
| d. | solutions with a pH between 5 and 9 | correct. These are thought to be safely administered into small peripheral veins with little risk of phlebitis |
Sources: Perry, A.G., Potter, P.A., & Ostendorf, W. (2017). Clinical skills and nursing techniques (9th ed). St. Louis, MO: Elsevier-Mosby.
Registered Nurses’ Association of Ontario (RNAO). (2005) Nursing best practice guideline: Care and maintenance to reduce vascular access complications [Revised 2008 supplement]. http://rnao.ca/sites/rnao-ca/files/Care_and_Maintenance_to_Reduce_Vascular_Access_Complications.pdf.
Media Attributions
- Svenska: Omläggning av PICC © Nurseirie is licensed under a CC BY-SA (Attribution ShareAlike) license
- Picture of my left hand and arm. © Michaelberry at English Wikipedia is licensed under a CC BY (Attribution) license
- Subclavian CVC © R. Anderson is licensed under a Public Domain license

