Atherosclerosis and Angina
Digestion and Absorption of Lipids
Karine Hamm
Learning Objectives
By the end of this chapter you will be able to:
- Describe the main steps of lipid digestion and absorption.
- Explain the importance of lipoproteins (low-density and high-density) in the context of atherosclerosis.
This chapter will discuss key steps of lipid digestion and absorption, which are essential for understanding the pathophysiology of atherosclerosis.
Lipids are large molecules and generally are not water-soluble. Like carbohydrates and protein, lipids are broken into small components for absorption. Since most of our digestive enzymes are water-based, how does the body break down fat and make it available for the various functions it must perform in the human body?
Please note that this chapter uses the words “lipids” and “fats” interchangeably.
From the Mouth to the Stomach
The process of lipid digestion begins in the mouth, where the action of chewing coupled with the action of a special enzyme (lingual lipase, which acts as an emulsifier) initiates the process. As a result, the fats become tiny droplets and separate from the watery components. Within two to four hours after eating a meal, roughly 30% of the triglycerides are converted to diglycerides and fatty acids by the stomach enzyme gastric lipase, yet very little fat digestion occurs in the stomach.
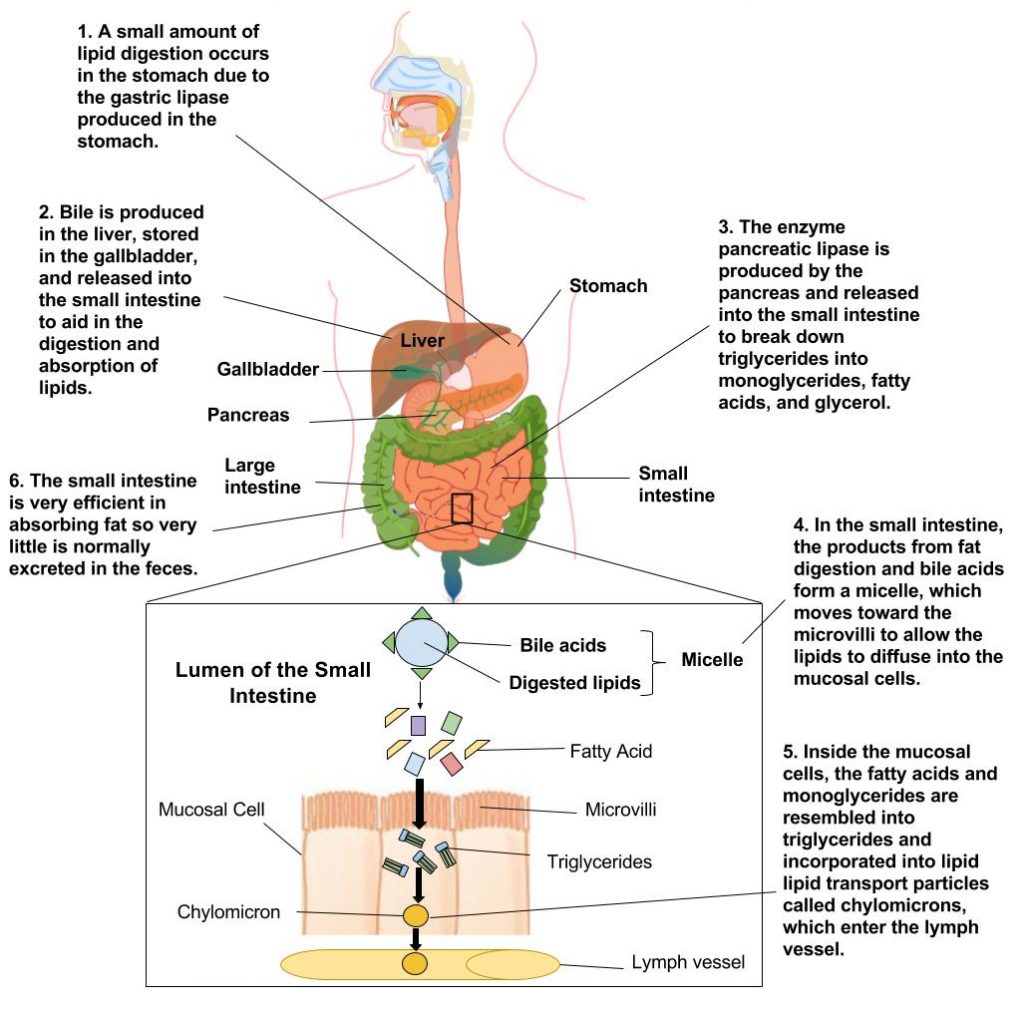
Going to the Bloodstream
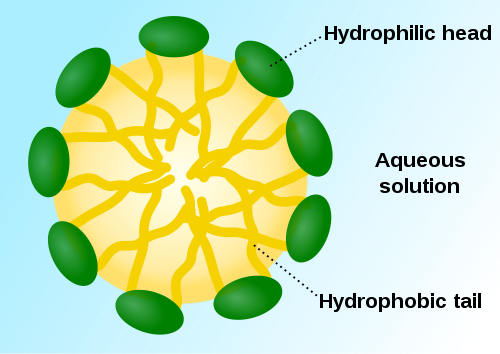
As stomach contents enter the small intestine, bile acts as an emulsifier and makes lipids more accessible to digestive enzymes, such as pancreatic lipase that breaks down the fats into free fatty acids and monoglycerides. Bile also facilitates the formation of micelles necessary for the transportation of fats through the lining of the digestive tract. Micelles have a fatty acid core with a water-soluble exterior. This allows efficient transportation to the intestinal microvillus, where the fat components are released and disseminated into the cells of the digestive tract lining.
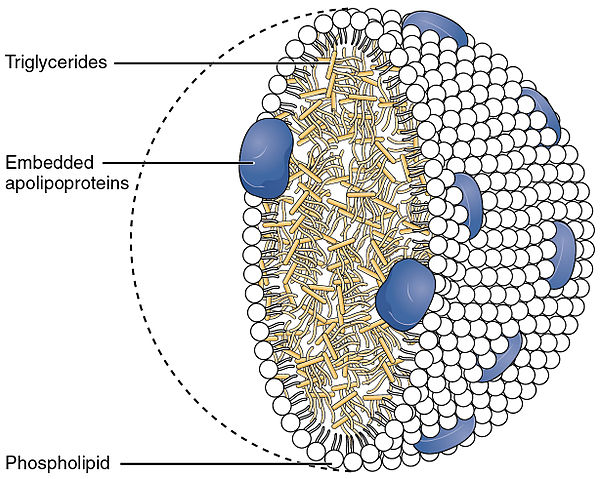
Within the lining of the digestive tract, monoglycerides and fatty acids reassemble into triglycerides that form lipoproteins when joined with a protein carrier. Lipoproteins have an inner core that is primarily made up of triglycerides and cholesterol esters (a cholesterol ester is a cholesterol linked to a fatty acid). The outer envelope is made of phospholipids interspersed with proteins and cholesterol. Together they form a chylomicron, which is a large lipoprotein that now enters the lymphatic system and will soon be released into the bloodstream via the jugular vein in the neck. Chylomicrons transport food fats perfectly through the body’s water-based environment to specific destinations such as the liver and other body tissues.
Understanding Blood Cholesterol
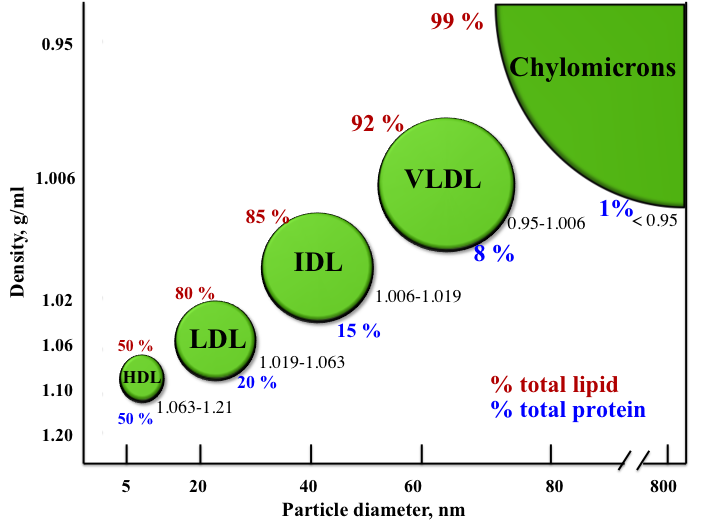
You may have heard of the abbreviations LDL and HDL with respect to heart health. These abbreviations refer to low-density lipoprotein (LDL) and high-density lipoprotein (HDL), respectively. Lipoproteins are characterized by size, density, and composition. As the size of the lipoprotein increases, the density decreases. This means that HDL is smaller than LDL. Why are they referred to as “good” and “bad” cholesterol?
Major Lipoproteins
Recall that chylomicrons are transporters of fats throughout the watery environment within the body. After about ten hours of circulating throughout the body, chylomicrons gradually release their triglycerides until all that is left of their composition is cholesterol-rich remnants. These remnants are used as raw materials by the liver to formulate specific lipoproteins. Following is a list of the various lipoproteins and their functions:
- VLDLs: Very low-density lipoproteins are made in the liver from remnants of chylomicrons and transport triglycerides from the liver to various tissues in the body. As the VLDLs travel through the circulatory system, the lipoprotein lipase strips the VLDL of triglycerides. As triglyceride removal persists, the VLDLs become intermediate-density lipoproteins.
- IDLs: Intermediate-density lipoproteins transport a variety of fats and cholesterol in the bloodstream and are a little under half triglyceride in composition. While traveling in the bloodstream, cholesterol is gained from other lipoproteins while circulating enzymes strip its phospholipid component. When IDLs return to the liver, they are transformed into low-density lipoprotein.
- LDLs: As low-density lipoproteins are commonly known as the “bad cholesterol” it is imperative that we understand their function in the body so as to make healthy dietary and lifestyle choices. LDLs carry cholesterol and other lipids from the liver to tissue throughout the body. LDLs are comprised of very small amounts of triglycerides, and house over 50 percent cholesterol and cholesterol esters. How does the body receive the lipids contained therein? As the LDLs deliver cholesterol and other lipids to the cells, each cell’s surface has receptor systems specifically designed to bind with LDLs. Circulating LDLs in the bloodstream bind to these LDL receptors and are consumed. Once inside the cell, the LDL is taken apart and its cholesterol is released. In liver cells these receptor systems aid in controlling blood cholesterol levels as they bind the LDLs. A deficiency of these LDL binding mechanisms will leave a high quantity of cholesterol traveling in the bloodstream, which can lead to heart disease or atherosclerosis. Diets rich in saturated fats will prohibit the LDL receptors which, are critical for regulating cholesterol levels.
- HDLs: High-density lipoproteins are responsible for carrying cholesterol out of the bloodstream and into the liver, where it is either reused or removed from the body with bile. HDLs have a very large protein composition coupled with low cholesterol content (20 to 30 percent) compared to the other lipoproteins. Hence, these high-density lipoproteins are commonly called “good cholesterol.”
Blood Cholesterol Considerations
For healthy total blood cholesterol, the desired range you would want to maintain is under 200 mg/dL. More specifically, when looking at individual lipid profiles, a low amount of LDL and a high amount of HDL prevents the excess buildup of cholesterol in the arteries and wards off potential health hazards. An LDL level of less than 100 milligrams per deciliter is ideal while an LDL level above 160 mg/dL would be considered high. In contrast, a low value of HDL is a telltale sign that a person is living with major risks for disease. Values of less than 40 mg/dL for men and 50 mg/dL for women mark a risk factor for developing heart disease. In short, elevated LDL blood lipid profiles indicate an increased risk of heart attack, while elevated HDL blood lipid profiles indicate a reduced risk.
Section Review
The process of lipid digestion involves multiple enzymes produced in different parts of the gastrointestinal tract (lingual lipase in the mouth, gastric lipase in the stomach, pancreatic lipase, and bile). Absorption of lipids happens primarily in the intestines, where lipids are combined with proteins to form lipoproteins – “vehicles” that can transport lipids in the bloodstream. In the context of atherosclerosis, two forms of lipoproteins (LDL of HDL) are of interest. LDLs, which transport lipid particles from the liver to the tissues/organs, are associated with an increased risk of atherosclerosis, while HDLs, which transport lipid particles from the tissue to the liver, are associated with a decreased risk. Smoking cessation, diets high in fiber and low in fat, and aerobic exercise increase the levels of HDL in the blood.
Review Questions
1. Finish the following sentence. Lipid absorption and digestion occur in the:
- Mouth
- Stomach
- Pancreas
- Intestines
2. Fill in the blank.
_____ is a general name of an enzyme that’s involved in lipid digestion.
3. Bile is produced by pancreas and secreted into small intestine to facilitate lipid digestion.
- True
- False
4. Fill in the blank.
Bile is produced by the _____ and acts as emulsifier to facilitate lipid digestion.
5. Fill in the blanks.
_____, also known as “bad cholesterol” is associated with increased risk of atherosclerosis. _____, or “good cholesterol”, is associated with lower risk of atherosclerosis initiation and progression.
Answer Key
- Intestines
- Lipase
- False
- Liver
- LDL, HDL
Attribution
Digestion and Absorption of Lipids by Karine Hamm is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License
Media Attributions
- Lipid-Digestion-and-absorption © Allison Calabrese is licensed under a CC BY (Attribution) license
- Micelle © Emmanuel Boutet is licensed under a CC BY (Attribution) license
- Chylomicron © Open Stax College is licensed under a CC BY (Attribution) license
- Lipoproteins © Karine Hamm is licensed under a CC BY (Attribution) license
A family of organic compounds composed of carbon, hydrogen, and oxygen. They are insoluble in water. The three main types of lipids are triglycerides, phospholipids, and sterols.
protein(s) that accelerate chemical reactions and transform substrate(s) into product(s)
a substtance that helps mix two liquids
The most common of the three basic classes of lipids and the main form fat takes in both diet and the human body. A triacylglycerol is made up of three molecules of fatty acids and one molecule of glycerol.
alkaline solution produced by the liver and important for the emulsification of lipids
an enzyme that breaks down fat
finger-like projection of the lining of the small intestine; a primary surface of nutrient absorption in the digestive system
a particle that consists a protein and a lipid (triglyceride or cholesterol). The main function of lipoproteins is to transport lipids through the bloodstream to various body tissues/organs
low-density lipoprotein, "bad cholesterol" , the form that carries lipids from the liver to various body tissue; increased levels of LDL can accumulate within the blood vessel wall and cause atherosclerosis
high-density lipoproteins, responsible for carrying cholesterol out of the bloodstream and into the liver; commonly referred to as "good cholesterol"

