Diabetes Mellitus
Diagnosis of Diabetes
Jennifer Kong
Learning Objectives
By the end of this section, you will be able to:
- Briefly describe some of the laboratory tests of diagnosing diabetes mellitus.
All types of diabetes mellitus are diagnosed most commonly using measurement of blood glucose levels.
In addition to taking a patient’s medical history (which highlights possible risk factors), the patient does a blood test with or without fasting (normal values are different).
- Random blood glucose test = blood is taken at any time of the day, regardless of whether the patient has eaten/drunk recently
- Fasting blood glucose test = blood is taken when a patient has not eaten/drunk for at least 8 hours. In healthy fasting patients, there should be normal glucose levels with low insulin.
If high blood glucose is detected, a subsequent test is performed in case the patient failed to follow instructions.
- Oral glucose tolerance test = patient is given a known amount of sugar to drink and then waits for 2h before blood sample is taken for glucose levels. In a patient without diabetes, insulin should be released to lower blood sugar levels down to normal. In a patient with diabetes, blood glucose levels will be high.
- Ketone test in blood or urine = the presence of ketones in the blood (draw blood) or urine (urine sample obtained in a cup) suggests that tissues are excessively using fat breakdown and not glucose for energy, possibly because insulin isn’t available.
- Hemoglobin A1C (glycosylated hemoglobin) = this blood test examines the values of blood glucose in the last 3 months. Red blood cells take up glucose, and since red blood cells live for less than 4 months, if blood glucose was high red blood cells accumulate the excess sugar that was exposed to them during those months. Specifically, the hemoglobin molecule will bind to glucose in a process called glycosylation. The hemoglobin will be more glycosylated only if exposed to excessive sugar in the 3-4 months of the red blood cell life.

|
Diagnosis of Diabetes Meeting ANY of the following criteria confirms diagnosis when classic symptoms of hyperglycemia are present Absence of classic symptoms of hyperglycemia requires a repeat confirmatory test |
|
| FPG ≥7.0 mmol/L |
|
| A1C ≥6.5% (in adults) |
|
| 2hPG in a 75 g OGTT ≥11.1 mmol/L | |
| Random PG ≥11.1 mmol/L in a patient with classic symptoms of hyperglycemia |
|
Section Review
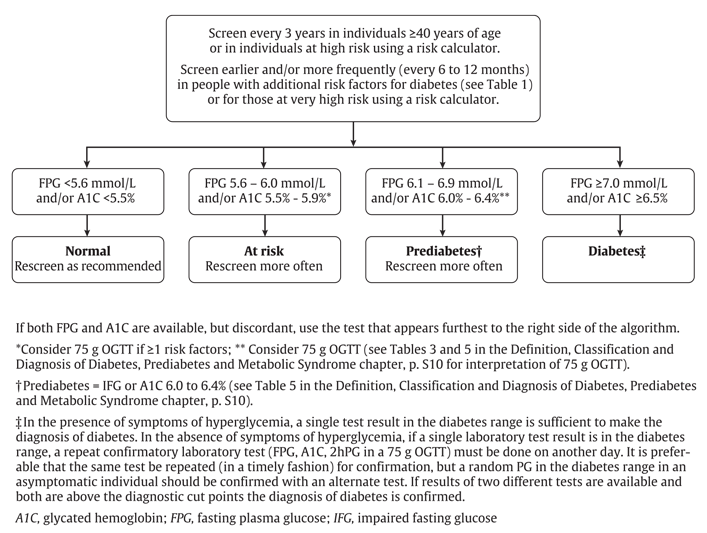
Diabetes is diagnosed through a blood test measuring glucose levels. Throughout the day, blood glucose levels fluctuate between 4-11 mmol/L depending on meals and activity. Hence, patients are instructed to not take in any nutrients (i.e. fast) for >8h to ensure – presumably – low levels of insulin with a normal range of blood glucose. If a patient’s fasting plasma glucose is above normal range (i.e. hyperglycemia), this indicates a lack of insulin response: whether due to lack of circulating insulin (T1DM) or resistance to insulin at the the tissue level (i.e. T2DM or gestational). If hyperglycemia is present for more than 3 months, the excess sugar will modify the red blood cells and can be detected by measuring glycosylated hemoglobin – known as “Hemoglobin A1C”. A further test for suspected diabetes is the oral glucose tolerance test (OGTT) where the patient ingests a known amount of sugar orally and their blood is measured 2h later. At this time, presumably, insulin levels will be at their highest with a decrease of blood glucose as the tissues respond to insulin. As blood high in glucose is being filtered by the kidney to produce urine, urine can be examined for the presence of glucose and/or ketones. Ketones will be present in both blood and urine if an abnormal amount of fat metabolism is occurring to compensate for the lack of glucose entering tissue for metabolism. When more than one test measures an inappropriately high amount of blood sugar/presence of ketones, diabetes mellitus is suspected and further investigations are needed to differentiate between the types of diabetes mellitus.
Optionally, check out Diabetes Canada‘s website where they outline screening for diabetes in adults.
Review Questions
1. Which of the following are tests taken to determine diabetes mellitus diagnoses? Select all that apply.
- Patient’s medical history
- Random blood glucose test
- Oral glucose tolerance test
- Hemoglobin A1C
- Lipid urine test
- Lipid blood test
- Fasting cholesterol blood test
- Iron blood test
2. Place the tests and definitions in the correct section – Preliminary Tests or Secondary Tests.
| Examining the glycosylation of sugar in red blood cells | Random Blood Glucose Test |
| Testing for the presence of ketones in blood or urine | Oral Glucose Tolerance Test |
| Blood taken at any time (regardless of most recent food/drink consumption) | Ketone Blood & Urine Test |
| Give known amount of sugar; wait 2 hours before taking blood sample | Fasting Blood Glucose Test |
| Blood taken without food/drink consumption 10 hours prior | Hemoglobin A1C |
| Preliminary Tests | Secondary Tests | ||
| Test | Definition | Test | Definition |
|
|
|||
|
|
|||
|
|
|||
3. If a patient is suspected to have diabetes mellitus, which of the following preliminary tests should they take to determine a diagnosis? Select all the apply.
- Random blood glucose test
- Fasting blood glucose test
- Oral glucose tolerance test
- Ketone urine test
- Ketone blood test
- Hemoglobin A1C
Answer Key
- Random blood glucose test, Oral glucose tolerance test, Ketone urine test, Hemoglobin A1C
- Review table below.
- Random blood glucose test, Fasting blood glucose test
| Preliminary Tests | Secondary Tests | ||
| Test | Definition | Test | Definition |
| Fasting Blood Glucose Test
|
Blood taken without food/drink consumption 10 hours prior |
Hemoglobin A1C
|
Examining the glycosylation of sugar in red blood cells |
| Random Blood Glucose Test | Blood taken at any time (regardless of most recent food/drink consumption) | Ketone Blood & Urine Test
|
Testing for the presence of ketones in blood or urine |
|
|
Oral Glucose Tolerance Test | Give known amount of sugar; wait 2 hours before taking blood sample | |
Media Attributions
Diabetes Canada Clinical Practice Guidelines Expert Committee. Diabetes Canada 2018 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada. Can J Diabetes. 2018;42(Suppl 1):S1-S325. [Internet]. [cited 2020 Oct 16]. Available from: http://guidelines.diabetes.ca/cpg
BC Guidelines for Diabetes Care https://www2.gov.bc.ca/gov/content/health/practitioner-professional-resources/bc-guidelines/diabetes#3
Media Attributions
- Hemoglobin A1c Test © Bruce Blaus is licensed under a CC BY (Attribution) license
- Diabetes screening-algorithm © BC Guidelines For Diabetes Care

