Emphysema
Organs and Structures of the Respiratory System
J. Gordon Betts; Kelly A. Young; James A. Wise; Eddie Johnson; Brandon Poe; Dean H. Kruse; Oksana Korol; Jody E. Johnson; Mark Womble; and Peter DeSaix
Learning Objectives
By the end of this section, you will be able to:
- List the structures that make up the respiratory system.
- Describe how the respiratory system processes oxygen and CO2.
- Compare and contrast the functions of upper respiratory tract with the lower respiratory tract.
The major organs of the respiratory system function primarily to provide oxygen to body tissues for cellular respiration, remove the waste product carbon dioxide, and help to maintain acid-base balance. Portions of the respiratory system are also used for non-vital functions, such as sensing odors, speech production, and for straining, such as during childbirth or coughing.
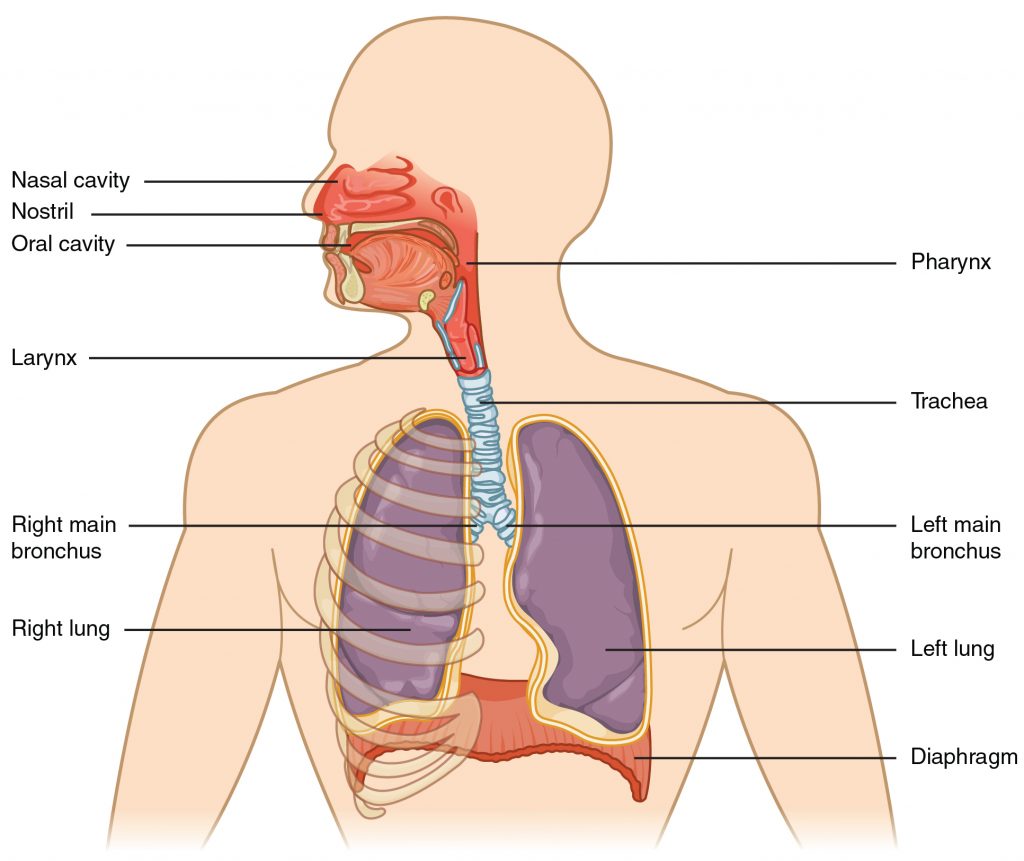
Functionally, the respiratory system can be divided into a conducting zone and a respiratory zone. The conducting zone of the respiratory system includes the organs and structures not directly involved in gas exchange. The gas exchange occurs in the respiratory zone.
Conducting Zone
The major functions of the conducting zone are to provide a route for incoming and outgoing air, remove debris and pathogens from the incoming air, and warm and humidify the incoming air. Several structures within the conducting zone perform other functions as well. The epithelium of the nasal passages, for example, is essential to sensing odors, and the bronchial epithelium that lines the lungs can metabolize some airborne carcinogens.
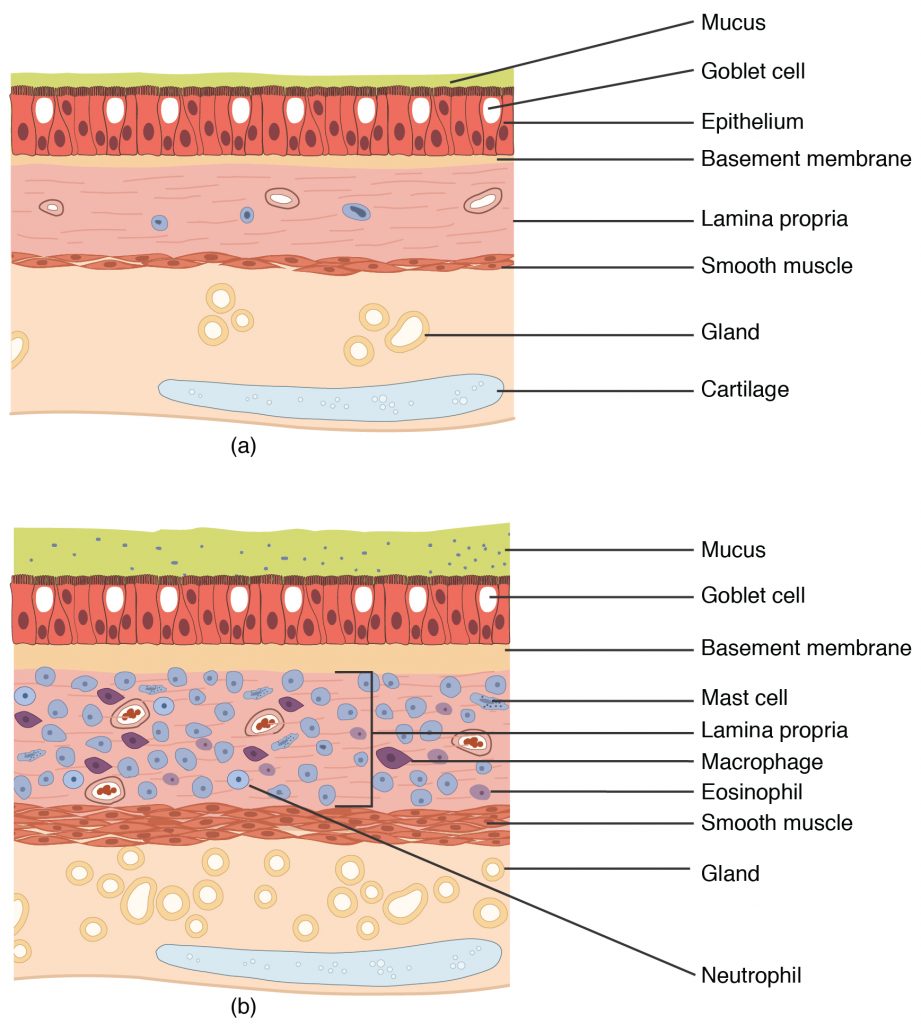
Aspects of the upper respiratory tract are lined byrespiratory epithelium composed of pseudostratified ciliated columnar epithelium. The epithelium contains goblet cells, one of the specialized, columnar epithelial cells that produce mucus to trap debris. The cilia of the respiratory epithelium help remove the mucus and debris with a constant beating motion, sweeping materials towards the throat to be swallowed. Interestingly, cold air slows the movement of the cilia, resulting in accumulation of mucus that may in turn lead to a runny nose during cold weather. This moist epithelium functions to warm and humidify incoming air. Capillaries located just beneath the nasal epithelium warm the air by convection. Serous and mucus-producing cells also secrete the lysozyme enzyme and proteins called defensins, which have antibacterial properties. Immune cells that patrol the connective tissue deep to the respiratory epithelium provide additional protection.
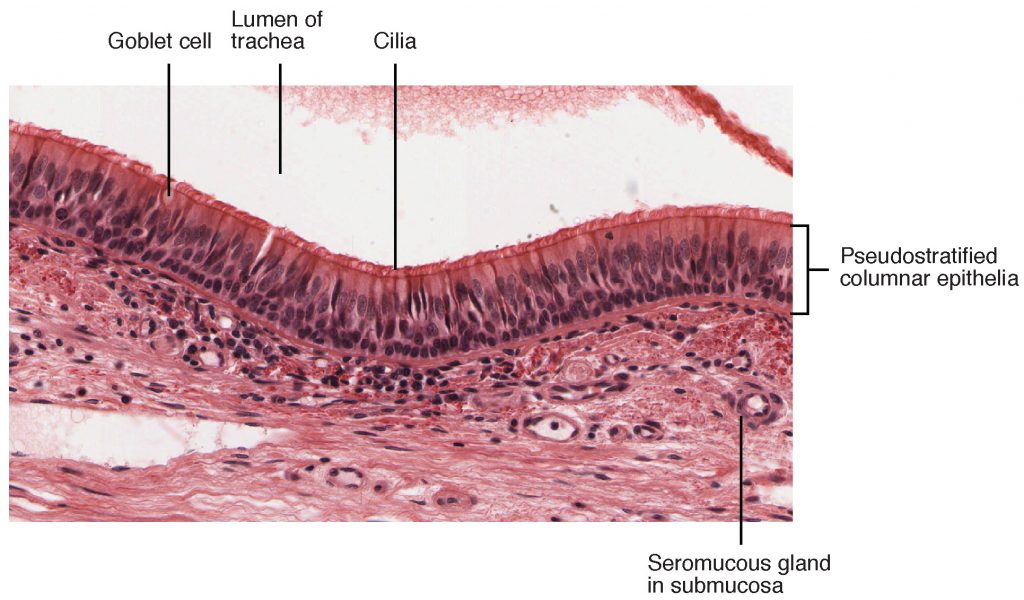
View the University of Michigan WebScope to explore the tissue sample in greater detail.
The trachea (windpipe) extends from the larynx toward the lungs. The trachea is formed by 16 to 20 stacked, C-shaped pieces of hyaline cartilage that are connected by dense connective tissue. The trachealis muscle and elastic connective tissue together form the fibroelastic membrane, a flexible membrane that closes the posterior surface of the trachea, connecting the C-shaped cartilages. The fibroelastic membrane allows the trachea to stretch and expand slightly during inhalation and exhalation, whereas the rings of cartilage provide structural support and prevent the trachea from collapsing. In addition, the trachealis muscle can be contracted to force air through the trachea during exhalation. The trachea is lined with pseudostratified ciliated columnar epithelium, which is continuous with the larynx. The esophagus borders the trachea posteriorly.
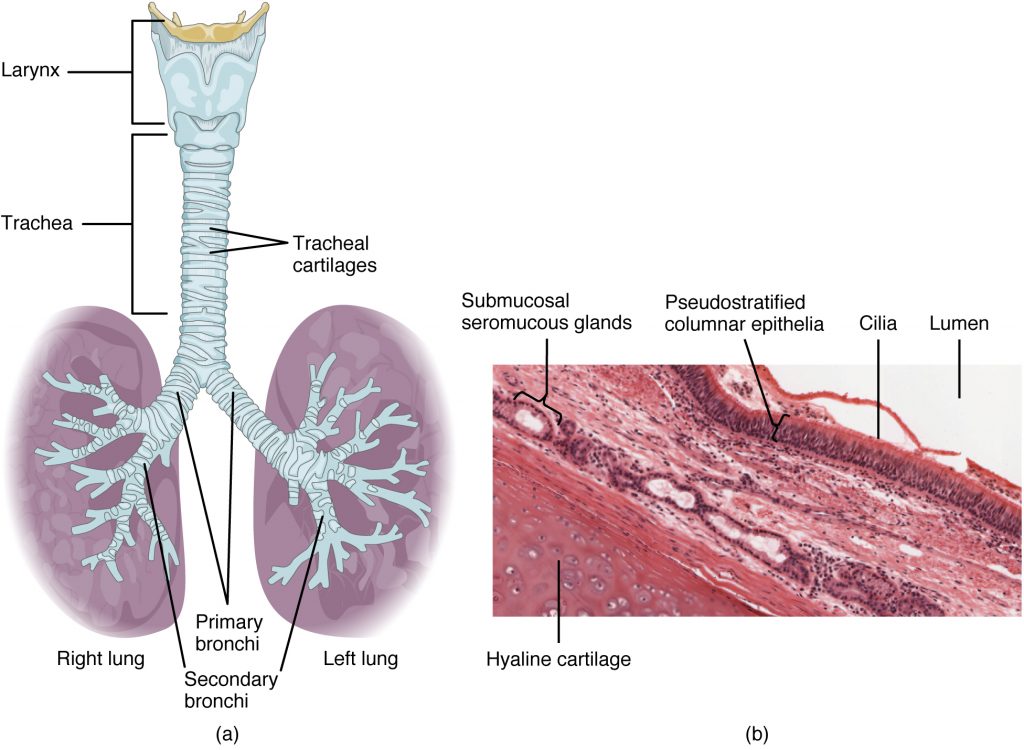
Bronchial Tree
The trachea branches into the right and left primary bronchi at the carina. These bronchi are also lined by pseudostratified ciliated columnar epithelium containing mucus-producing goblet cells. The carina is a raised structure that contains specialized nervous tissue that induces violent coughing if a foreign body, such as food, is present. Rings of cartilage, similar to those of the trachea, support the structure of the bronchi and prevent their collapse. The primary bronchi enter the lungs at the hilum, a concave region where blood vessels, lymphatic vessels, and nerves also enter the lungs. The bronchi continue to branch into bronchial a tree. A bronchial tree (or respiratory tree) is the collective term used for these multiple-branched bronchi. The main function of the bronchi, like other conducting zone structures, is to provide a passageway for air to move into and out of each lung. In addition, the mucous membrane traps debris and pathogens.
A bronchiole branches from the tertiary bronchi. Bronchioles, which are about 1 mm in diameter, further branch until they become the tiny terminal bronchioles, which lead to the structures of gas exchange. There are more than 1000 terminal bronchioles in each lung. The muscular walls of the bronchioles do not contain cartilage like those of the bronchi. This muscular wall can change the size of the tubing to increase or decrease airflow through the tube.
Respiratory Zone
In contrast to the conducting zone, the respiratory zone includes structures that are directly involved in gas exchange. The respiratory zone begins where the terminal bronchioles join a respiratory bronchiole, the smallest type of bronchiole, which then leads to an alveolar duct, opening into a cluster of alveoli.
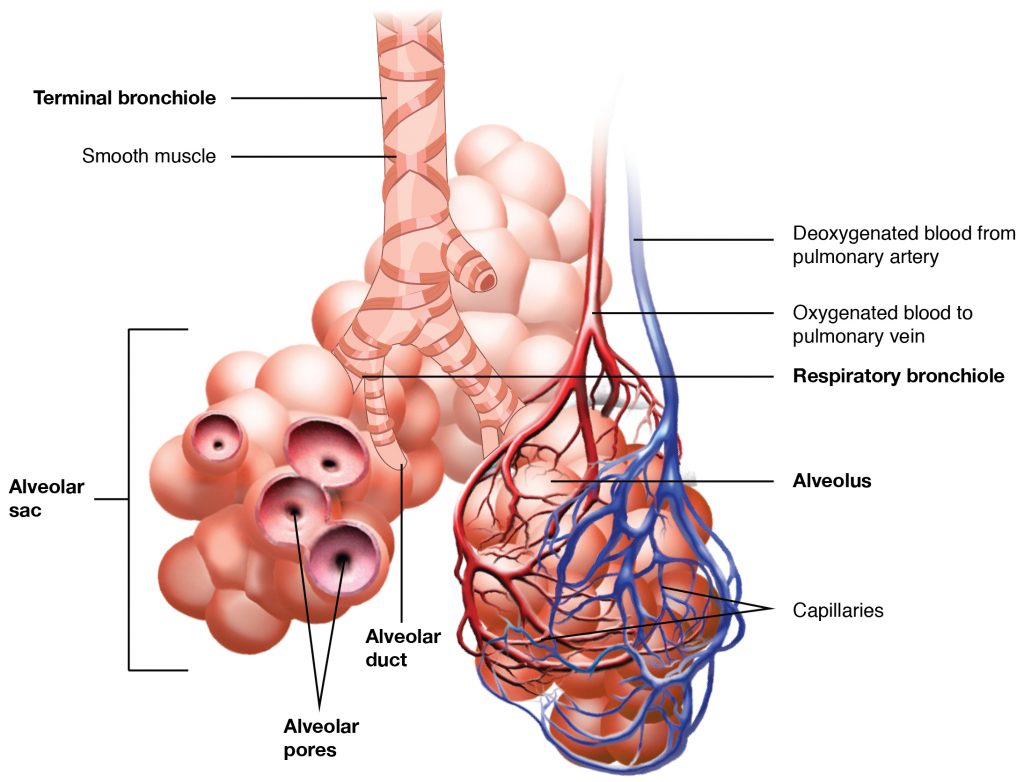
Alveoli
An alveolar duct is a tube composed of smooth muscle and connective tissue, which opens into a cluster of alveoli. An alveolus is one of the many small, grape-like sacs that are attached to the alveolar ducts.
An alveolar sac is a cluster of many individual alveoli that are responsible for gas exchange. An alveolus is approximately 200 μm in diameter with elastic walls that allow the alveolus to stretch during air intake, which greatly increases the surface area available for gas exchange. Alveoli are connected to their neighbors by alveolar pores, which help maintain equal air pressure throughout the alveoli and lung.
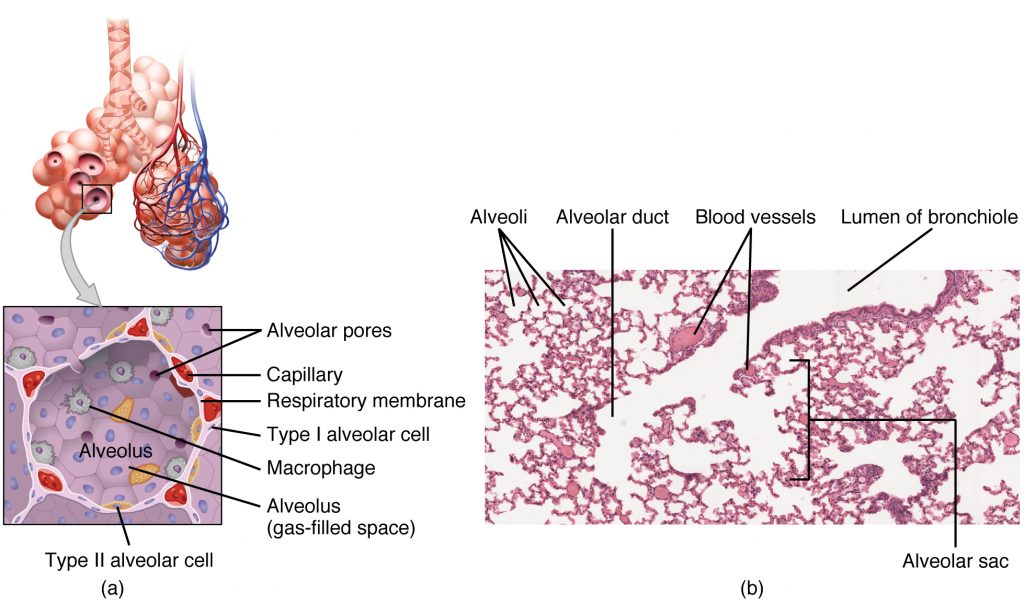
The alveolar wall consists of three major cell types: type I alveolar cells, type II alveolar cells, and alveolar macrophages. A type I alveolar cell is a squamous epithelial cell of the alveoli, which constitute up to 97 percent of the alveolar surface area. These cells are about 25 nm thick and are highly permeable to gases. A type II alveolar cell is interspersed among the type I cells and secretes pulmonary surfactant, a substance composed of phospholipids and proteins that reduces the surface tension of the alveoli. Roaming around the alveolar wall is the alveolar macrophage, a phagocytic cell of the immune system that removes debris and pathogens that have reached the alveoli.
The simple squamous epithelium formed by type I alveolar cells is attached to a thin, elastic basement membrane. This epithelium is extremely thin and borders the endothelial membrane of capillaries. Taken together, the alveoli and capillary membranes form a respiratory membrane that is approximately 0.5 μm (micrometers) thick. The respiratory membrane allows gases to cross by simple diffusion, allowing oxygen to be picked up by the blood for transport and CO2 to be released into the air of the alveoli.
Diseases of the Respiratory System: Asthma
Asthma is common condition that affects the lungs in both adults and children. Approximately 8.2 percent of adults (18.7 million) and 9.4 percent of children (7 million) in the United States suffer from asthma. In addition, asthma is the most frequent cause of hospitalization in children.
Asthma is a chronic disease characterized by inflammation and edema of the airway, and bronchospasms (that is, constriction of the bronchioles), which can inhibit air from entering the lungs. In addition, excessive mucus secretion can occur, which further contributes to airway occlusion. Cells of the immune system, such as eosinophils and mononuclear cells, may also be involved in infiltrating the walls of the bronchi and bronchioles.
Bronchospasms occur periodically and lead to an “asthma attack.” An attack may be triggered by environmental factors such as dust, pollen, pet hair, or dander, changes in the weather, mold, tobacco smoke, and respiratory infections, or by exercise and stress.
Symptoms of an asthma attack involve coughing, shortness of breath, wheezing, and tightness of the chest. Symptoms of a severe asthma attack that requires immediate medical attention would include difficulty breathing that results in blue (cyanotic) lips or face, confusion, drowsiness, a rapid pulse, sweating, and severe anxiety. The severity of the condition, frequency of attacks, and identified triggers influence the type of medication that an individual may require. Longer-term treatments are used for those with more severe asthma. Short-term, fast-acting drugs that are used to treat an asthma attack are typically administered via an inhaler. For young children or individuals who have difficulty using an inhaler, asthma medications can be administered via a nebulizer.
In many cases, the underlying cause of the condition is unknown. However, recent research has demonstrated that certain viruses, such as human rhinovirus C (HRVC), and the bacteria Mycoplasma pneumoniae and Chlamydia pneumoniae that are contracted in infancy or early childhood, may contribute to the development of many cases of asthma.
Visit this video on how airway size is involved in asthma to learn more about what happens during an asthma attack. What are the three changes that occur inside the airways during an asthma attack?
Section Review
The respiratory system is responsible for obtaining oxygen and getting rid of carbon dioxide, and aiding in speech production and in sensing odors. From a functional perspective, the respiratory system can be divided into two major areas: the conducting zone and the respiratory zone. The conducting zone consists of all of the structures that provide passageways for air to travel into and out of the lungs: the nasal cavity, pharynx, trachea, bronchi, and most bronchioles. The nasal passages contain the conchae and meatuses that expand the surface area of the cavity, which helps to warm and humidify incoming air, while removing debris and pathogens. The pharynx is composed of three major sections: the nasopharynx, which is continuous with the nasal cavity; the oropharynx, which borders the nasopharynx and the oral cavity; and the laryngopharynx, which borders the oropharynx, trachea, and esophagus. The respiratory zone includes the structures of the lung that are directly involved in gas exchange: the terminal bronchioles and alveoli.
The lining of the conducting zone is composed mostly of pseudostratified ciliated columnar epithelium with goblet cells. The mucus traps pathogens and debris, whereas beating cilia move the mucus superiorly toward the throat, where it is swallowed. As the bronchioles become smaller and smaller, and nearer the alveoli, the epithelium thins and is simple squamous epithelium in the alveoli. The endothelium of the surrounding capillaries, together with the alveolar epithelium, forms the respiratory membrane. This is a blood-air barrier through which gas exchange occurs by simple diffusion.
Review Questions
1. Which of the following anatomical structures is not part of the conducting zone?
- Pharynx
- Nasal cavity
- Alveoli
- Bronchi
2. Which of the following are structural features of the trachea? Select all that apply.
- C-shaped cartilage
- Smooth muscle fibres
- Cilia
- None of the above
3. What is the role of alveolar macrophages?
- To secrete antimicrobial proteins
- To remove pathogens and debris
- To facilitate gas exchange
- To secrete pulmonary surfactant
4. Compare and contrast the conducting and respiratory zone.
Answer Key
- Alveoli
- C-shaped cartilage
- To remove pathogens and debris
- The conducting zone includes the organs and structures that are not directly involved in gas exchange, but perform other duties such as providing a passageway for air, trapping and removing debris and pathogens, and warming and humidifying incoming air. Such structures include the nasal cavity, pharynx, larynx, trachea, and most of the bronchial tree. The respiratory zone includes all the organs and structures that are directly involved in gas exchange, including the respiratory bronchioles, alveolar ducts, and alveoli.
References
Bizzintino J, Lee WM, Laing IA, Vang F, Pappas T, Zhang G, Martin AC, Khoo SK, Cox DW, Geelhoed GC, et al. Association between human rhinovirus C and severity of acute asthma in children. Eur Respir J [Internet]. 2010 [cited 2013 Mar 22]; 37(5):1037–1042. Available from: http://erj.ersjournals.com/gca?submit=Go&gca=erj%3B37%2F5%2F1037&allch=
Kumar V, Ramzi S, Robbins SL. Robbins Basic Pathology. 7th ed. Philadelphia (PA): Elsevier Ltd; 2005.
Martin RJ, Kraft M, Chu HW, Berns, EA, Cassell GH. A link between chronic asthma and chronic infection. J Allergy Clin Immunol [Internet]. 2001 [cited 2013 Mar 22]; 107(4):595-601. Available from: http://erj.ersjournals.com/gca?submit=Go&gca=erj%3B37%2F5%2F1037&allch=
Adaption
This chapter is adapted from the following text:
Organs and structures of respiratory system in Anatomy and Physiology by OSCRiceUniversity is licensed under a Creative Commons Attribution 4.0 International License
Media Attributions
- 2301_Major_Respiratory_Organs © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2304_Pseudostratified_Epithelium © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2308_The_Trachea © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2309_The_Respiratory_Zone © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2310_Structures_of_the_Respiratory_Zone © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2311_Lung_Tissue © OSCRiceUniversity is licensed under a CC BY (Attribution) license
Region of the respiratory system that includes the organs and structures that provide passageways for air and are not directly involved in gas exchange.
Includes structures of the respiratory system that are directly involved in gas exchange.
Ciliated lining of much of the conducting zone that is specialized to remove debris and pathogens, and produce mucus.
Tube composed of cartilaginous rings and supporting tissue that connects the lung bronchi and the larynx; provides a route for air to enter and exit the lung.
Cartilaginous structure that produces the voice, prevents food and beverages from entering the trachea, and regulates the volume of air that enters and leaves the lungs.
Smooth muscle located in the fibroelastic membrane of the trachea.
Specialized membrane that connects the ends of the C-shape cartilage in the trachea; contains smooth muscle fibers.
Collective name for the multiple branches of the bronchi and bronchioles of the respiratory system.
Branch of bronchi that are 1 mm or less in diameter and terminate at alveolar sacs.
Specific type of bronchiole that leads to alveolar sacs.
Small tube that leads from the terminal bronchiole to the respiratory bronchiole and is the point of attachment for alveoli.
Small, grape-like sac that performs gas exchange in the lungs.
Cluster of alveoli.
Opening that allows airflow between neighboring alveoli.
Squamous epithelial cells that are the major cell type in the alveolar wall; highly permeable to gases.
Cuboidal epithelial cells that are the minor cell type in the alveolar wall; secrete pulmonary surfactant.
Immune system cell of the alveolus that removes debris and pathogens.
Substance composed of phospholipids and proteins that reduces the surface tension of the alveoli; made by type II alveolar cells.
Alveolar and capillary wall together, which form an air-blood barrier that facilitates the simple diffusion of gases.
Region of the conducting zone that forms a tube of skeletal muscle lined with respiratory epithelium; located between the nasal conchae and the esophagus and trachea.
One of three recesses (superior, middle, and inferior) in the nasal cavity attached to the conchae that increase the surface area of the nasal cavity.
Portion of the pharynx flanked by the conchae and oropharynx that serves as an airway.
Portion of the pharynx flanked by the nasopharynx, oral cavity, and laryngopharynx that is a passageway for both air and food.
Portion of the pharynx bordered by the oropharynx superiorly and esophagus and trachea inferiorly; serves as a route for both air and food.

