Pneumonia and Pulmonary Edema
Diagnosis and Treatment of Pneumonia
Simon Duffy and Jennifer Kong
Learning Objectives
By the end of this section, you will be able to:
- Relate pathophysiology with clinical diagnosis of pneumonia.
- Briefly describe what X-ray is and how it is used in the diagnosis of pneumonia.
- Briefly describe what microbiology testing (medical laboratory sciences) is and how it is used in the diagnosis of pneumonia.
- Describe common treatment options for pneumonia.
Diagnosis of Pneumonia: Physical Examination
The lungs are not immediately visible because they are contained inside the chest cavity. However, a clinical professional can use their senses of sight, hearing, and touch in order to get clues for possible infection.
The sense of sight can be used to observe a patient’s breathing. A person with pneumonia may not be getting enough oxygen, resulting this the need for a more rapid respiration rate (tachypnea). Also, this person will breath using muscles not normally engaged during breathing, called accessory muscles. The patient is working harder to breathe and may also complain of this sensation (dyspnea).
The sense of hearing can be used when performing auscultation (with or without percussion) during a physical exam. Listening for signs of infection – and when it happens during inhalation/exhalation – will involve the use of a stethoscope (auscultation). For example, the thick, sticky exudate in pneumonia may cause the lung to make abnormal sounds upon auscultation: a ‘course crackle” in the affected lung. Percussion is tapping on the affected area of the chest. When listening during percussion, the flow of air can be easily heard during inhalation and exhalation. However, in pneumonia, the exudate – being mostly fluid – will dampen sound, resulting in a ‘dull” or diminished breath sounds during auscultation. Auscultation while the patient is speaking can also help during examination. When a person speaks, the vocalizations may be transmitted more efficiently in the fluid that builds up within the lung. (recall that sound travels better in water than in air). Hence, these vocalizations will sound louder than normal using the stethoscope on the affected side.
The sense of touch can involve palpation, the process of using hands and fingers in order to feel evidence of illness. In normal breathing, you feel equal respiratory expansion on both sides of the body. However, in lobar pneumonia a whole section of the lung is not functioning and you would feel an asymmetric during chest expansion.
Diagnosis of Pneumonia: Medical Imaging (X-ray)
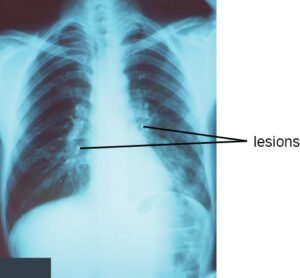
Consolidation of the lung can be easily visualized by X-ray. Recall that X-rays will make air-filled structures (like the lung) as black (radioluscent). However, the production of exudate in pneumonia (i.e. consolidation) will show up as white (radioopaque). Any abnormalities in the X-ray are defined as ‘lesions’. Hence, X-rays are a fast and easily accessible method to determine the location and extent of consolidation.
Listen to Michelle Beauchamp, a medical radiography technologist (X-ray), introduce how X-rays work. She explains the experience a patient with pneumonia (possibly due to heart failure complications) will have when coming in for a chest X-ray. She speaks about the important role medical radiography plays in a health care team in diagnosis of a disease. She also shares a fun fact about the diverse work environments of a medical radiography technologists!
Medical Radiography (X-Ray) created by Michelle Beauchamp & Jennifer Kong, licensed under CC-BY-NC
Diagnosis of Pneumonia: Sputum Analysis
Sputum is the mucus that is coughed up from the lower airways of the respiratory tract, and can have many clues for a possible infection. The sputum colour may be informative. For example, a yellow or green colour may result from immune cells forming as pus within the airway. A rusty, pink or red colour may reflect blood-tinged sputum due to infectious exudate.
Visual inspection of sputum may not be enough to confirm infection, so sputum may be cultured in a laboratory to grow and analyze the microbes in it. Few microbes should grow in the lung sputum and the culture is considered positive when the number of microbes exceeds a safe range. Lab tests can aim to identify whether known pathogens are present in order to guide clinical decisions. In addition to a microbial culture to grow microbes, the microbes may be tested for sensitivity to antimicrobials (e.g. antibiotics). Culture & Sensitivity testing is an important step in selecting the most effective therapy for a patient.
Listen to Marion Regan, a medical laboratory technologist (microbiology), introduce her field and subspecialties. She speak about the journey the sputum specimen (from a patient with suspected pneumonia) takes from collection to identification. She also describes the important role of medical laboratory science in a health care team as their tests aid in the diagnosis of diseases. She also shares a fun fact about what it’s like to work in a medical laboratory facility!
Medical Laboratory Sciences (Microbiology) and Pneumonia created by Marion Regan & Jennifer Kong, licensed under CC-BY-NC
Diagnosis of Pneumonia: Blood Analysis
Blood tests can be used to generally assess a person’s health by looking at the body’s response to infection and the expected ensuing inflammatory response. A complete blood count (CBC) measures the overproduction of immune cells that may be due to infection. Erythrocyte sedimentation rate (ESR) is based on a phenomenon where red blood cells become more dense when people experience inflammation. Some blood molecules, such as C-reactive protein (CRP) and pro-calcitonin can be measured at high amount during inflammation. Blood oxygen levels may also be measured using methods like pulse oximetry. If the lung is not functioning properly, the content of oxygen in the blood might decrease while carbon dioxide levels may rise.
Blood tests can also monitor for potentially harmful infections of the blood, called septicemia. These involve culture and sensitivity tests, described in the sputum analysis section above. Infections of the bloodstream must be carefully managed because they can result in a severe immune response, called sepsis. Sepsis is the body’s extreme response to infection, where there is a chain reaction of inflammation throughout the body. Due to the severity of this immune response, sepsis can rapidly lead to permanent tissue damage, organ failure and even death.
Treatment of Pneumonia
Treatment of pneumonia depends largely on what microbe is involved in the infection as well as how the illness presents. As well, treatment must also include methods to help the patient’s feeling of dyspnea and lessen the effort of breathing during pneumonia. Until C&S results determine the specific antimicrobial, the health care team may implement changes to aid breathing. Medications can be given to help widen airways and, if necessary, dampen the swelling in airways due to inflammation. The best method to deliver this medication is through metered dose inhalers – more commonly known as ‘puffers’. Similarly, if consolidation is significant enough to decrease gas exchange, blood oxygenation will be decreased and assessed with a pulse oximeter. If blood oxygen saturation becomes less than 95%, extra oxygen may be inhaled to enrich each breath during inspiration.
Interprofessional Collaboration During Diagnosis and Treatment of Pneumonia
As you can imagine, there is a large health care team involved when treating someone with pneumonia – especially if they have comorbidities and/or are hospitalized. Please read the following patient case studies to get a glimpse of the members of this health care team.
Listen to author Simon Duffy’s interview with nurse Anna Kornienko as she describes her experience caring for a patient with pneumonia and coordinating patient access with the members of the health care team.
Nursing management of pneumonia. Created by chapter author Simon Duffy and nurse Anna Kornienko, licensed under CC-BY-NC
Section Review
- A physical examination involving observation of breathing patterns, breathing sounds and palpation can provide evidence for pneumonia.
- Medical radiography technologists take X-rays, a type of radiation which helps visualize the body based on a tissue’s density which can stop X-rays (radiopaque) or not (radiolucent). Chest X-rays allow for visualization of the size of the heart and whether there is fluid in the lungs – useful in the diagnosis of pneumonia.
- Microbiology, a specialty of medical laboratory science, can analyze blood and sputum samples to determine the identity of the pathogen which is causing infection and the antimicrobials which can treat the infection (e.g. antibiotics). Microbiology is integral to a primary care provider to choosing the appropriate antimicrobial to treat the pneumonia
- Treatment of pneumonia involves antimicrobials to manage the infection but also medications to support breathing and tissue oxygenation.
Review Questions
1. Which of the following statements is NOT true in regards to chest X-rays?
- X-rays use ionizing radiation to image the body for the diagnosis or monitoring of injury or disease.
- X-rays pass easily through air and are stopped by dense substances like bone.
- Patients undergoing a chest X-ray will typically have two images taken at 90 degrees of one another, to help make sure nothing is missed.
- When looking at a chest X-ray, normal lung will appear as white (radioopaque) while consolidated sections of lung will appear as black (radioluscent).
2. Which of the following could point towards a case of pneumonia? Select all that apply.
- A yellow/green or rusty colour to the patient’s sputum sample
- A culture from patient sputum with a number of microbes below the threshold
- Blood tests show that the patient has a high complete blood count (CBC) and erythrocyte sedimentation rate (ESR)
- Chest X-ray showing multiple lesions throughout the lung
3. Explain how physical examination, medical imaging, sputum analysis, and blood analysis all contribute to the management of a patient with suspected pneumonia. Think about how a test might contribute to diagnosis or treatment.
Answer Key
- When looking at a chest X-ray, normal lung will appear as white (radioopaque) while consolidated sections of lung will appear as black (radioluscent).
- A yellow/green or rusty colour to the patient’s sputum sample, blood tests show that the patient has a high complete blood count (CBC) and erythrocyte sedimentation rate (ESR), chest X-ray showing multiple lesions throughout the lung
Media Attributions
- OSC_Microbio_22_02_Pneumonia © OSCRiceUniversity is licensed under a CC BY (Attribution) license
rapid and shallow breathing; respiratory rate is >21 breaths per minute in adults
a feeling of not being able to breathe well enough; short of breath
listening with a stethoscope for changes in sounds produced by movement of air, blood, food digestion, etc.

