Emphysema
Inflammation and Fever
Nina Parker; Mark Schneegurt; Anh-Hue Thi Tu; Philip Lister; and Brian M. Forster
Learning Objectives
At the end of this section, you will be able to:
- Identify the signs of inflammation and fever and explain why they occur.
- Explain the advantages and risks posed by inflammatory responses.
The inflammatory response, or inflammation, is triggered by a cascade of chemical mediators and cellular responses that may occur when cells are damaged and stressed or when pathogens successfully breach the physical barriers of the innate immune system. Although inflammation is typically associated with negative consequences of injury or disease, it is a necessary process insofar as it allows for recruitment of the cellular defenses needed to eliminate pathogens, remove damaged and dead cells, and initiate repair mechanisms. Excessive inflammation, however, can result in local tissue damage and, in severe cases, may even become deadly.
Acute Inflammation
An early, if not immediate, response to tissue injury is acute inflammation. Immediately following an injury, vasoconstriction of blood vessels will occur to minimize blood loss. The amount of vasoconstriction is related to the amount of vascular injury, but it is usually brief. Vasoconstriction is followed by vasodilation and increased vascular permeability, as a direct result of the release of histamine from resident mast cells. Increased blood flow and vascular permeability can dilute toxins and bacterial products at the site of injury or infection. They also contribute to the five observable signs associated with the inflammatory response: erythema (redness), edema, heat, pain, and altered function. Vasodilation and increased vascular permeability are also associated with an influx of phagocytes at the site of injury and/or infection. This can enhance the inflammatory response because phagocytes may release proinflammatory chemicals when they are activated by cellular distress signals released from damaged cells, by PAMPs , or by opsonins on the surface of pathogens. Activation of the complement system can further enhance the inflammatory response through the production of the anaphylatoxin C5a. The image below illustrates a typical case of acute inflammation at the site of a skin wound.
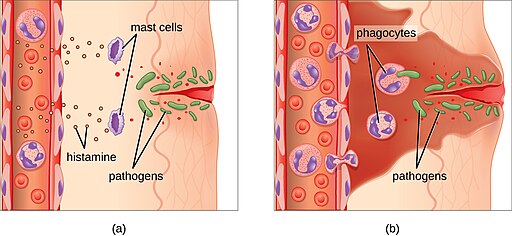
During the period of inflammation, the release of bradykinin causes capillaries to remain dilated, flooding tissues with fluids and leading to edema. Increasing numbers of neutrophils are recruited to the area to fight pathogens. As the fight rages on, pus forms from the accumulation of neutrophils, dead cells, tissue fluids, and lymph. Typically, after a few days, macrophages will help to clear out this pus. Eventually, tissue repair can begin in the wounded area.
Chronic Inflammation
When acute inflammation is unable to clear an infectious pathogen, chronic inflammation may occur. This often results in an ongoing (and sometimes futile) lower-level battle between the host organism and the pathogen. The wounded area may heal at a superficial level, but pathogens may still be present in deeper tissues, stimulating ongoing inflammation. Additionally, chronic inflammation may be involved in the progression of degenerative neurological diseases such as Alzheimer’s and Parkinson’s, heart disease, and metastatic cancer.
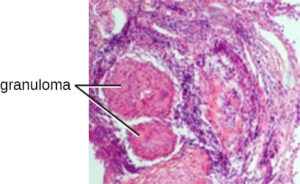
Chronic inflammation may lead to the formation of granulomas, pockets of infected tissue walled off and surrounded by WBCs. Macrophages and other phagocytes wage an unsuccessful battle to eliminate the pathogens and dead cellular materials within a granuloma. One example of a disease that produces chronic inflammation is tuberculosis, which results in the formation of granulomas in lung tissues. A tubercular granuloma is called a tubercle.
Chronic inflammation is not just associated with bacterial infections. Chronic inflammation can be an important cause of tissue damage from viral infections. The extensive scarring observed with hepatitis C infections and liver cirrhosis is the result of chronic inflammation.
Chronic Edema
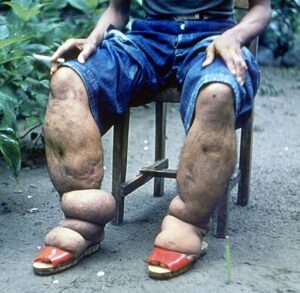
In addition to granulomas, chronic inflammation can also result in long-term edema. A condition known as lymphatic filariasis (also known as elephantiasis) provides an extreme example. Lymphatic filariasis is caused by microscopic nematodes (parasitic worms) whose larvae are transmitted between human hosts by mosquitoes. Adult worms live in the lymphatic vessels, where their presence stimulates infiltration by lymphocytes, plasma cells, eosinophils, and thrombocytes (a condition known as lymphangitis). Because of the chronic nature of the illness, granulomas, fibrosis, and blocking of the lymphatic system may eventually occur. Over time, these blockages may worsen with repeated infections over decades, leading to skin thickened with edema and fibrosis. Lymph (extracellular tissue fluid) may spill out of the lymphatic areas and back into tissues, causing extreme swelling. Secondary bacterial infections commonly follow. Because it is a disease caused by a parasite, eosinophilia (a dramatic rise in the number of eosinophils in the blood) is characteristic of acute infection. However, this increase in antiparasite granulocytes is not sufficient to clear the infection in many cases.
Lymphatic filariasis affects an estimated 120 million people worldwide, mostly concentrated in Africa and Asia.[1] Improved sanitation and mosquito control can reduce transmission rates.
Fever
A fever is an inflammatory response that extends beyond the site of infection and affects the entire body, resulting in an overall increase in body temperature. Body temperature is normally regulated and maintained by the hypothalamus, an anatomical section of the brain that functions to maintain homeostasis in the body. However, certain bacterial or viral infections can result in the production of pyrogens, chemicals that effectively alter the “thermostat setting” of the hypothalamus to elevate body temperature and cause fever. Pyrogens may be exogenous or endogenous. For example, the endotoxin lipopolysaccharide (LPS), produced by gram-negative bacteria, is an exogenous pyrogen that may induce the leukocytes to release endogenous pyrogens such as interleukin-1 (IL-1), IL-6, interferon-γ (IFN-γ), and tumour necrosis factor (TNF). In a cascading effect, these molecules can then lead to the release of prostaglandin E2 (PGE2) from other cells, resetting the hypothalamus to initiate fever.
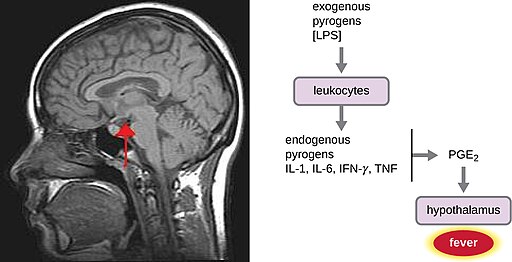
Like other forms of inflammation, a fever enhances the innate immune defenses by stimulating leukocytes to kill pathogens. The rise in body temperature also may inhibit the growth of many pathogens since human pathogens have optimum growth occurring around 35 °C (95 °F). In addition, some studies suggest that fever may also stimulate release of iron-sequestering compounds from the liver, thereby starving out microbes that rely on iron for growth.[2]
During fever, the skin may appear pale due to vasoconstriction of the blood vessels in the skin, which is mediated by the hypothalamus to divert blood flow away from extremities, minimizing the loss of heat and raising the core temperature. The hypothalamus will also stimulate shivering of muscles, another effective mechanism of generating heat and raising the core temperature.
The crisis phase occurs when the fever breaks. The hypothalamus stimulates vasodilation, resulting in a return of blood flow to the skin and a subsequent release of heat from the body. The hypothalamus also stimulates sweating, which cools the skin as the sweat evaporates.
Although a low-level fever may help an individual overcome an illness, in some instances, this immune response can be too strong, causing tissue and organ damage and, in severe cases, even death. The inflammatory response to bacterial superantigens is one scenario in which a life-threatening fever may develop. Superantigens are bacterial or viral proteins that can cause an excessive activation of T cells from the specific adaptive immune defense, as well as an excessive release of cytokines that overstimulates the inflammatory response. For example, Staphylococcus aureus and Streptococcus pyogenes are capable of producing superantigens that cause toxic shock syndrome and scarlet fever, respectively. Both of these conditions can be associated with very high, life-threatening fevers in excess of 42 °C (108 °F).
Section Review
- Inflammation results from the collective response of chemical mediators and cellular defenses to an injury or infection.
- Acute inflammation is short lived and localized to the site of injury or infection. Chronic inflammation occurs when the inflammatory response is unsuccessful, and may result in the formation of granulomas (e.g., with tuberculosis) and scarring (e.g., with hepatitis C viral infections and liver cirrhosis).
- The five cardinal signs of inflammation are erythema, edema, heat, pain, and altered function. These largely result from innate responses that draw increased blood flow to the injured or infected tissue.
- Fever is a system-wide sign of inflammation that raises the body temperature and stimulates the immune response.
- Both inflammation and fever can be harmful if the inflammatory response is too severe.
Review Questions
1. Which refers to swelling as a result of inflammation?
- Erythema
- Edema
- Granuloma
- Vasodilation
2. Which type of inflammation occurs at the site of an injury or infection?
- Acute
- Chronic
- Endogenous
- Exogenous
3. Fill in the blank.
A(n) _____ is a walled-off area of infected tissue that exhibits chronic inflammation.
4. Fill in the blank.
The _____ is the part of the body responsible for regulating body temperature.
5. Fill in the blank.
Heat and redness, or _____, occur when the small blood vessels in an inflamed area dilate (open up), bringing more blood much closer to the surface of the skin.
6. Name the five stages of inflammation.
Answer Key
- Edema
- Acute
- Granuloma
- Hypothalamus
- Erythema
- Heat, redness, swelling (erythema), pain, and altered function
Adaption
This chapter is adapted from the following text:
Inflammation and fever in Microbiology by Rice University (OpenStax) is licensed under a Creative Commons Attribution 4.0 International License
Media Attributions
- 512px-OSC_Microbio_17_06_Erythema © CNX OpenStax is licensed under a CC BY (Attribution) license
- Granuloma © CNX OpenStax is licensed under a CC BY (Attribution) license
- 512px-OSC_Microbio_17_06_Elephant © CNX OpenStax is licensed under a CC BY (Attribution) license
- 512px-OSC_Microbio_17_06_Hypothal © CNX OpenStax is licensed under a CC BY (Attribution) license
a necessary process that recruits the cellular defenses needed to eliminate pathogens, remove damaged and dead cells, and initiate repair mechanisms
inflammatory response that occurs from the time of injury to infection up to a few days
constriction of the smooth muscle of a blood vessel, resulting in a decreased vascular diameter
relaxation of the smooth muscle in the wall of a blood vessel, resulting in an increased vascular diameter
increased blood in tissue, resulting in visible redness and increased heat
'swelling' of tissue, most often due to increased fluid in the interstitial spaces
Pathogen-associated molecular patterns are small molecular motifs conserved within a class of microbes.
extracellular proteins that mark it to be be phagocytosed
a pro-inflammatory peptide with many vasoactive and inflammatory effects
a protein-rich fluid formed at the site of inflammation during bacterial or fungal infection. Filled with dead cells and leukocytes, pus is typically white-yellow, yellow, or yellow-brown.
a slow, long-term inflammation, in response to repeated injury, lasting for weeks, months to years.
pockets of infected tissue walled off and surrounded by white blood cells
an infectious bacterial disease (usually caused by Mycobacterium tuberculosis bacteria) that generally affects the lungs, but can also affect other parts of the body
parasitic worms that live in the lymphatic vessels causing a chronic inflammatory response. This results in blockage of lymph flow causing edema, repeated infections, skin thickening and fibrosis.
a systemic inflammatory response that extends beyond the site of infection and affects the entire body, resulting in an overall increase in body temperature
chemicals that effect the temperature set point in the hypothalamus, thus elevating body temperature and causing fever.
part of the brain below the thalamus that is an important interface between the central nervous system and vasculature. Amongst its many functions, it plays a major role in hormonal secretion, temperature and fluid homeostasis, and emotional regulation.
bacterial or viral proteins that can cause an excessive inflammatory response

