Atherosclerosis and Angina
Blood Flow and Blood Pressure
J. Gordon Betts; Kelly A. Young; James A. Wise; Eddie Johnson; Brandon Poe; Dean H. Kruse; Oksana Korol; Jody E. Johnson; Mark Womble; and Peter DeSaix
Learning Objectives
By the end of this section, you will be able to:
- Distinguish between systolic pressure, diastolic pressure, pulse pressure, and mean arterial pressure.
- Describe the clinical measurement of blood pressure.
- Identify and discuss five variables affecting arterial blood flow and blood pressure.
Blood flow refers to the movement of blood through a vessel, tissue, or organ, and is usually expressed in terms of volume of blood per unit of time. It is initiated by the contraction of the ventricles of the heart. Ventricular contraction ejects blood into the major arteries, resulting in flow from regions of higher pressure to regions of lower pressure, as blood encounters smaller arteries and arterioles, then capillaries, then the venules and veins of the venous system. This section discusses a number of critical variables that contribute to blood flow throughout the body. It also discusses the factors that impede or slow blood flow, a phenomenon known as resistance.
As noted earlier, hydrostatic pressure is the force exerted by a fluid due to gravitational pull, usually against the wall of the container in which it is located. One form of hydrostatic pressure is blood pressure, the force exerted by blood upon the walls of the blood vessels or the chambers of the heart. Blood pressure may be measured in capillaries and veins, as well as the vessels of the pulmonary circulation; however, the term blood pressure without any specific descriptors typically refers to systemic arterial blood pressure—that is, the pressure of blood flowing in the arteries of the systemic circulation. In clinical practice, this pressure is measured in mm Hg and is usually obtained using the brachial artery of the arm.
Components of Arterial Blood Pressure
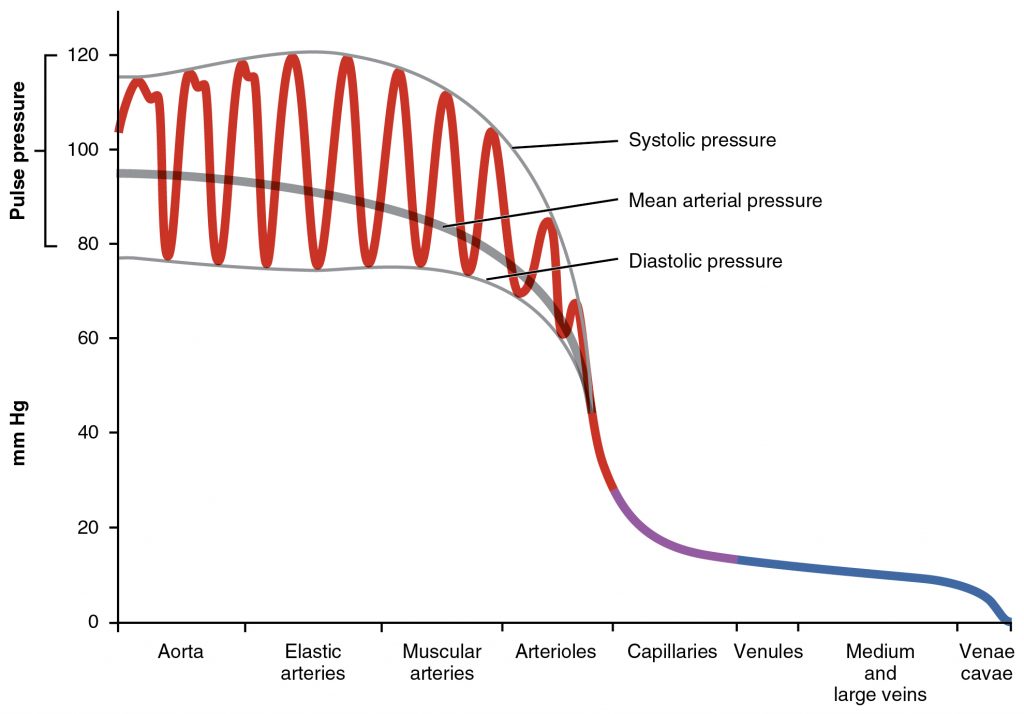
Arterial blood pressure in the larger vessels consists of several distinct components: systolic and diastolic pressures, pulse pressure, and mean arterial pressure.
Systolic and Diastolic Pressures
When systemic arterial blood pressure is measured, it is recorded as a ratio of two numbers (e.g., 120/80 is a normal adult blood pressure), expressed as systolic pressure over diastolic pressure. The systolic pressure is the higher value (typically around 120 mm Hg) and reflects the arterial pressure resulting from the ejection of blood during ventricular contraction, or systole. The diastolic pressure is the lower value (usually about 80 mm Hg) and represents the arterial pressure of blood during ventricular relaxation, or diastole.
Measurement of Blood Pressure
Blood pressure is one of the critical parameters measured on virtually every patient in every healthcare setting. The technique used today was developed more than 100 years ago by a pioneering Russian physician, Dr. Nikolai Korotkoff. Turbulent blood flow through the vessels can be heard as a soft ticking while measuring blood pressure; these sounds are known as Korotkoff sounds. The technique of measuring blood pressure requires the use of a sphygmomanometer (a blood pressure cuff attached to a measuring device) and a stethoscope. The technique is as follows:
- The clinician wraps an inflatable cuff tightly around the patient’s arm at about the level of the heart.
- The clinician squeezes a rubber pump to inject air into the cuff, raising pressure around the artery and temporarily cutting off blood flow into the patient’s arm.
- The clinician places the stethoscope on the patient’s antecubital region and, while gradually allowing air within the cuff to escape, listens for the Korotkoff sounds.
Although there are five recognized Korotkoff sounds, only two are normally recorded. Initially, no sounds are heard since there is no blood flow through the vessels, but as air pressure drops, the cuff relaxes, and blood flow returns to the arm. As shown below, the first sound heard through the stethoscope—the first Korotkoff sound—indicates systolic pressure. As more air is released from the cuff, blood is able to flow freely through the brachial artery and all sounds disappear. The point at which the last sound is heard is recorded as the patient’s diastolic pressure.
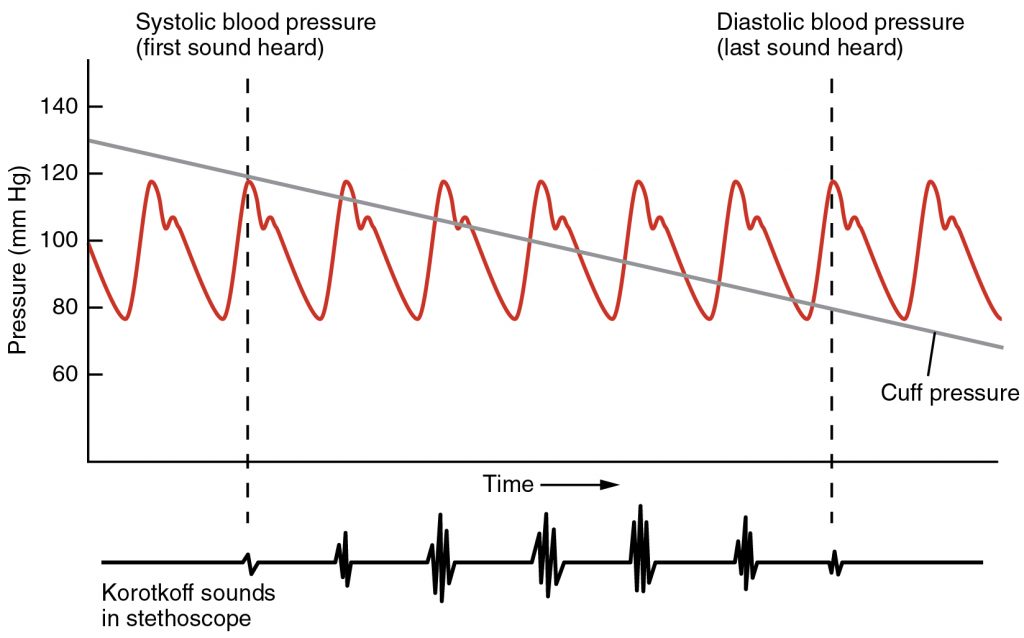
The majority of hospitals and clinics have automated equipment for measuring blood pressure that work on the same principles. An even more recent innovation is a small instrument that wraps around a patient’s wrist. The patient then holds the wrist over the heart while the device measures blood flow and records pressure.
Variables Affecting Blood Flow and Blood Pressure
Five variables influence blood flow and blood pressure:
- Cardiac output: increase in heart rate or stroke volume will elevate blood pressure and promote blood flow, decrease in cardiac output will decrease arterial pressure and blood flow.
- Compliance: veins are more compliant than arteries and can expand to hold more blood. Stiffness of arteris due to vascular disease reduces compliance and increases pressure within the vessel. This also increases the work of the heart.
- Volume of the blood – hypovolemia (can be caused by bleeding, dehydration, vomiting, etc) lowers blood pressure, hypervolemia (can be caused by heart failure, liver cirrhosis, kidney disease) elevates blood pressure.
- Viscosity of the blood – determined by formed elements (erythrocytes, etc) and plasma proteins. Anemia or liver conditions can decrease viscosity, decrease resistance, and increase blood flow.
- Blood vessel length and diameter – the length of a vessel is directly proportional to its resistance: the longer the vessel, the greater the resistance and the lower the flow. The effect of diameter on resistance is inversely related to the resistance and flow.
Section Review
Blood flow is the movement of blood through a vessel, tissue, or organ. The slowing or blocking of blood flow is called resistance. Blood pressure is the force that blood exerts upon the walls of the blood vessels or chambers of the heart. The components of blood pressure include systolic pressure, which results from ventricular contraction, and diastolic pressure, which results from ventricular relaxation. Pulse pressure is the difference between systolic and diastolic measures, and mean arterial pressure is the “average” pressure of blood in the arterial system, driving blood into the tissues. Pulse, the expansion and recoiling of an artery, reflects the heartbeat. The variables affecting blood flow and blood pressure in the systemic circulation are cardiac output, compliance, blood volume, blood viscosity, and the length and diameter of the blood vessels. In the arterial system, vasodilation and vasoconstriction of the arterioles is a significant factor in systemic blood pressure: Slight vasodilation greatly decreases resistance and increases flow, whereas slight vasoconstriction greatly increases resistance and decreases flow. In the arterial system, as resistance increases, blood pressure increases and flow decreases. In the venous system, constriction increases blood pressure as it does in arteries; the increasing pressure helps to return blood to the heart. In addition, constriction causes the vessel lumen to become more rounded, decreasing resistance and increasing blood flow. Venoconstriction, while less important than arterial vasoconstriction, works with the skeletal muscle pump, the respiratory pump, and their valves to promote venous return to the heart.
Review Questions
1. In a blood pressure measurement of 110/70, the number 70 is the:
- Systolic pressure
- Diastolic pressure
- Pulse pressure
- Mean arterial pressure
2. A healthy elastic artery:
- Is compliant
- Reduces blood flow
- Is a resistance artery
- Has a thin wall and irregular lumen
3. Increased heart rate can result in increased blood pressure.
- True
- False
4. Fill in the blanks.
_____ of arteries due to vascular disease or atherosclerosis can _____ blood pressure.
Answer Key
- Diastolic pressure
- Is compliant
- True
- Stiffness, increase/elevate
Adaption
This chapter is adapted from the following text:
Blood flow, pressure & resistance in Anatomy and Physiology by OSCRiceUniversity is licensed under a Creative Commons Attribution 4.0 International License
Media Attributions
- 2109_Systemic_Blood_Pressure © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2111_Blood_Pressure_Graph © OSCRiceUniversity is licensed under a CC BY (Attribution) license
movement of blood through a vessel, tissue, or organ that is usually expressed in terms of volume per unit of time
one of the primary pumping chambers of the heart located in the lower portion of the heart; the left ventricle is the major pumping chamber on the lower left side of the heart that ejects blood into the systemic circuit via the aorta and receives blood from the left atrium; the right ventricle is the major pumping chamber on the lower right side of the heart that ejects blood into the pulmonary circuit via the pulmonary trunk and receives blood from the right atrium
any condition or parameter that slows or counteracts the flow of blood
force exerted by the blood against the wall of a vessel or heart chamber; can be described with the more generic term hydrostatic pressure
a part of the heart cycle; contraction of the heart ventricles that ejects blood out of the heart
relaxation of ventricles during the cardiac cycle
blood pressure cuff attached to a device that measures blood pressure
larger number recorded when measuring arterial blood pressure; represents the maximum value following ventricular contraction
lower number recorded when measuring arterial blood pressure; represents the minimal value corresponding to the pressure that remains during ventricular relaxation
measurement of blood flow from the heart through the ventricles, is usually measured in liters per minute
amount of blood ejected from the ventricle with each cardiac cycle
degree to which a blood vessel can stretch as opposed to being rigid
decrease in blood volume
abnormally high levels of fluid and blood within the body
thickness of fluids that affects their ability to flow

