Preface
Epithelial Tissue
J. Gordon Betts; Kelly A. Young; James A. Wise; Eddie Johnson; Brandon Poe; Dean H. Kruse; Oksana Korol; Jody E. Johnson; Mark Womble; and Peter DeSaix
Learning Objectives
This section gives the background of how many cells make up epithelial tissue and key features. This background will be instrumental for the subsequent videos of histological examination of normal and pathological tissue. By the end of this section, you will be able to:
- Explain the structure and function of epithelial tissue.
- Distinguish between tight junctions, anchoring junctions, and gap junctions.
- Distinguish between simple epithelia and stratified epithelia, as well as between squamous, cuboidal, and columnar epithelia.
- Describe the structure and function of endocrine and exocrine glands and their respective secretions.
Most epithelial tissues are essentially large sheets of cells covering all the surfaces of the body exposed to the outside world and lining the outside of organs. Epithelium also forms much of the glandular tissue of the body. Skin is not the only area of the body exposed to the outside. Other areas include the airways, the digestive tract, as well as the urinary and reproductive systems, all of which are lined by an epithelium. Hollow organs and body cavities that do not connect to the exterior of the body, which includes, blood vessels and serous membranes, are lined by endothelium (plural = endothelia), which is a type of epithelium.
All epithelia share some important structural and functional features. This tissue is highly cellular, with little or no extracellular material present between cells. Adjoining cells form a specialized intercellular connection between their cell membranes called a cell junction. The epithelial cells exhibit polarity with differences in structure and function between the exposed or apical facing surface of the cell and the basal surface close to the underlying body structures. The basal lamina, a mixture of glycoproteins and collagen, provides an attachment site for the epithelium, separating it from underlying connective tissue. The basal lamina attaches to a reticular lamina, which is secreted by the underlying connective tissue, forming a basement membrane that helps hold it all together.
Epithelial tissues are nearly completely avascular. For instance, no blood vessels cross the basement membrane to enter the tissue, and nutrients must come by diffusion or absorption from underlying tissues or the surface. Many epithelial tissues are capable of rapidly replacing damaged and dead cells. Sloughing off of damaged or dead cells is a characteristic of surface epithelium and allows our airways and digestive tracts to rapidly replace damaged cells with new cells.
Generalized Functions of Epithelial Tissue
Epithelial tissues provide the body’s first line of protection from physical, chemical, and biological wear and tear. The cells of an epithelium act as gatekeepers of the body controlling permeability and allowing selective transfer of materials across a physical barrier. All substances that enter the body must cross an epithelium. Some epithelia often include structural features that allow the selective transport of molecules and ions across their cell membranes.
Many epithelial cells are capable of secretion and release mucous and specific chemical compounds onto their apical surfaces. The epithelium of the small intestine releases digestive enzymes, for example. Cells lining the respiratory tract secrete mucous that traps incoming microorganisms and particles. A glandular epithelium contains many secretory cells.
The Epithelial Cell
Epithelial cells are typically characterized by the polarized distribution of organelles and membrane-bound proteins between their basal and apical surfaces. Particular structures found in some epithelial cells are an adaptation to specific functions. Certain organelles are segregated to the basal sides, whereas other organelles and extensions, such as cilia, when present, are on the apical surface.
Cilia are microscopic extensions of the apical cell membrane that are supported by microtubules. They beat in unison and move fluids as well as trapped particles. Ciliated epithelium lines the ventricles of the brain where it helps circulate the cerebrospinal fluid. The ciliated epithelium of your airway forms a mucociliary escalator that sweeps particles of dust and pathogens trapped in the secreted mucous toward the throat. It is called an escalator because it continuously pushes mucous with trapped particles upward. In contrast, nasal cilia sweep the mucous blanket down towards your throat. In both cases, the transported materials are usually swallowed, and end up in the acidic environment of your stomach.
Cell to Cell Junctions
Cells of epithelia are closely connected and are not separated by intracellular material. Three basic types of connections allow varying degrees of interaction between the cells: tight junctions, anchoring junctions, and gap junctions.
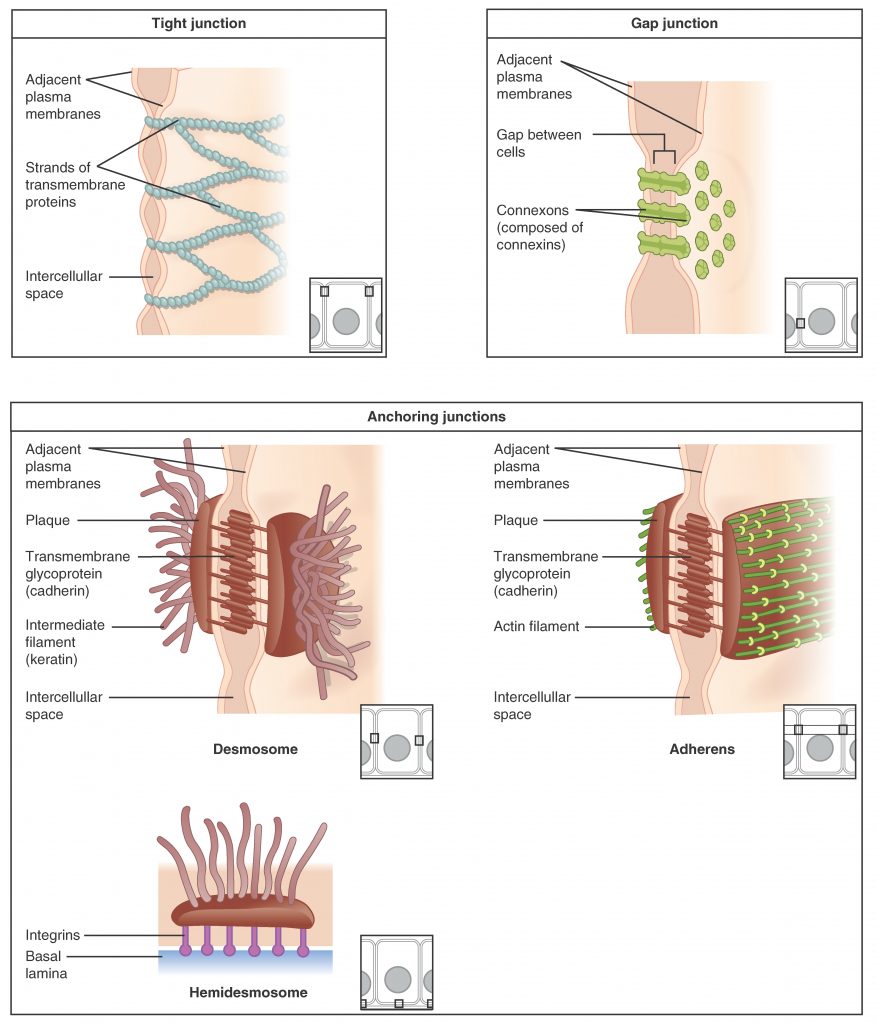
At one end of the spectrum is the tight junction, which separates the cells into apical and basal compartments. When two adjacent epithelial cells form a tight junction, there is no extracellular space between them and the movement of substances through the extracellular space between the cells is blocked. This enables the epithelia to act as selective barriers. An anchoring junction includes several types of cell junctions that help stabilize epithelial tissues. Anchoring junctions are common on the lateral and basal surfaces of cells where they provide strong and flexible connections. These junctions influence the shape and folding of the epithelial tissue.
In contrast with the tight and anchoring junctions, a gap junction forms an intercellular passageway between the membranes of adjacent cells to facilitate the movement of small molecules and ions between the cytoplasm of adjacent cells. These junctions allow electrical and metabolic coupling of adjacent cells, which coordinates function in large groups of cells.
Classification of Epithelial Tissues
Epithelial tissues are classified according to the shape of the cells and number of the cell layers formed. Cell shapes can be squamous (flattened and thin), cuboidal (boxy, as wide as it is tall), or columnar (rectangular, taller than it is wide). Similarly, the number of cell layers in the tissue can be one—where every cell rests on the basal lamina—which is a simple epithelium, or more than one, which is a stratified epithelium and only the basal layer of cells rests on the basal lamina. Pseudostratified (pseudo- = “false”) describes tissue with a single layer of irregularly shaped cells that give the appearance of more than one layer. Transitional describes a form of specialized stratified epithelium in which the shape of the cells can vary.
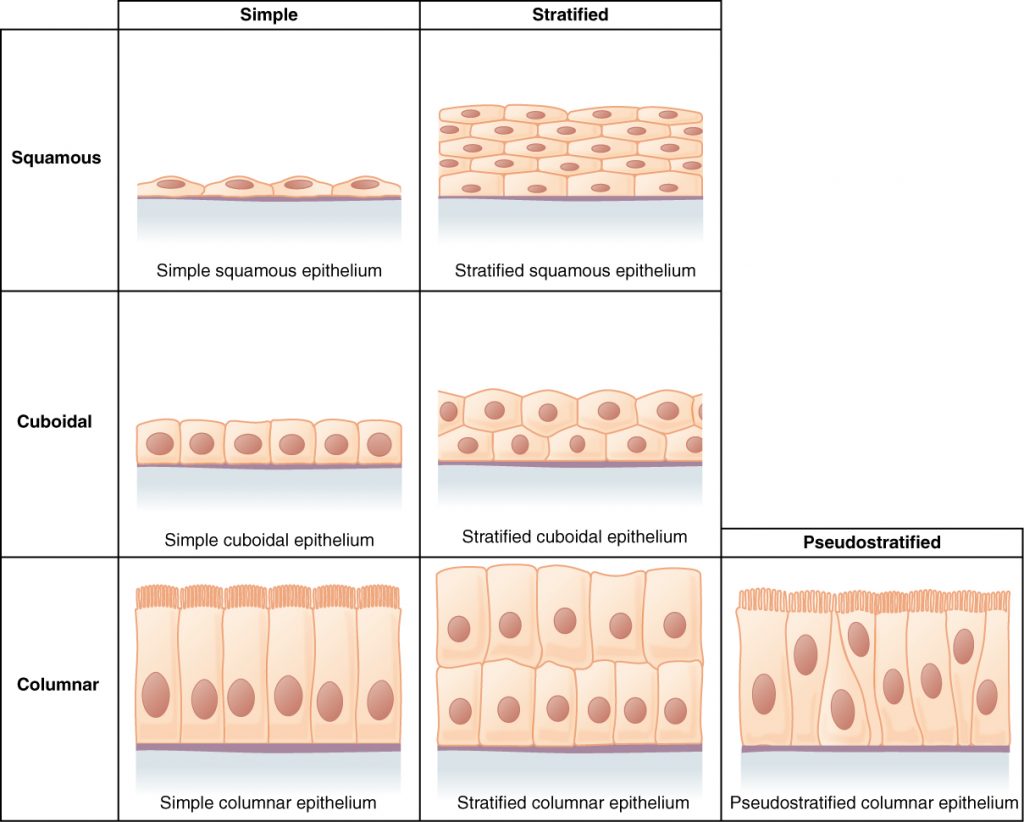
Simple Epithelium
The shape of the cells in the single cell layer of simple epithelium reflects the functioning of those cells. The cells in simple squamous epithelium have the appearance of thin scales. Squamous cell nuclei tend to be flat, horizontal, and elliptical, mirroring the form of the cell. The endothelium is the epithelial tissue that lines vessels of the lymphatic and cardiovascular system, and it is made up of a single layer of squamous cells. Simple squamous epithelium, because of the thinness of the cell, is present where rapid passage of chemical compounds is observed. The alveoli of lungs where gases diffuse, segments of kidney tubules, and the lining of capillaries are also made of simple squamous epithelial tissue. The mesothelium is a simple squamous epithelium that forms the surface layer of the serous membrane that lines body cavities and internal organs. Its primary function is to provide a smooth and protective surface.
In simple cuboidal epithelium, the nucleus of the box-like cells appears round and is generally located near the center of the cell. These epithelia are active in the secretion and absorptions of molecules. Simple cuboidal epithelia are observed in the lining of the kidney tubules and in the ducts of glands.
In simple columnar epithelium, the nucleus of the tall column-like cells tends to be elongated and located in the basal end of the cells. Like the cuboidal epithelia, this epithelium is active in the absorption and secretion of molecules. Simple columnar epithelium forms the lining of some sections of the digestive system and parts of the female reproductive tract. Ciliated columnar epithelium is composed of simple columnar epithelial cells with cilia on their apical surfaces. These epithelial cells are found in the lining of the fallopian tubes and parts of the respiratory system, where the beating of the cilia helps remove particulate matter.
Pseudostratified columnar epithelium is a type of epithelium that appears to be stratified but instead consists of a single layer of irregularly shaped and differently sized columnar cells. In pseudostratified epithelium, nuclei of neighboring cells appear at different levels rather than clustered in the basal end. The arrangement gives the appearance of stratification; but in fact all the cells are in contact with the basal lamina, although some do not reach the apical surface. Pseudostratified columnar epithelium is found in the respiratory tract, where some of these cells have cilia.
Both simple and pseudostratified columnar epithelia are heterogeneous epithelia because they include additional types of cells interspersed among the epithelial cells. For example, a goblet cell is a mucous-secreting unicellular “gland” interspersed between the columnar epithelial cells of mucous membranes.
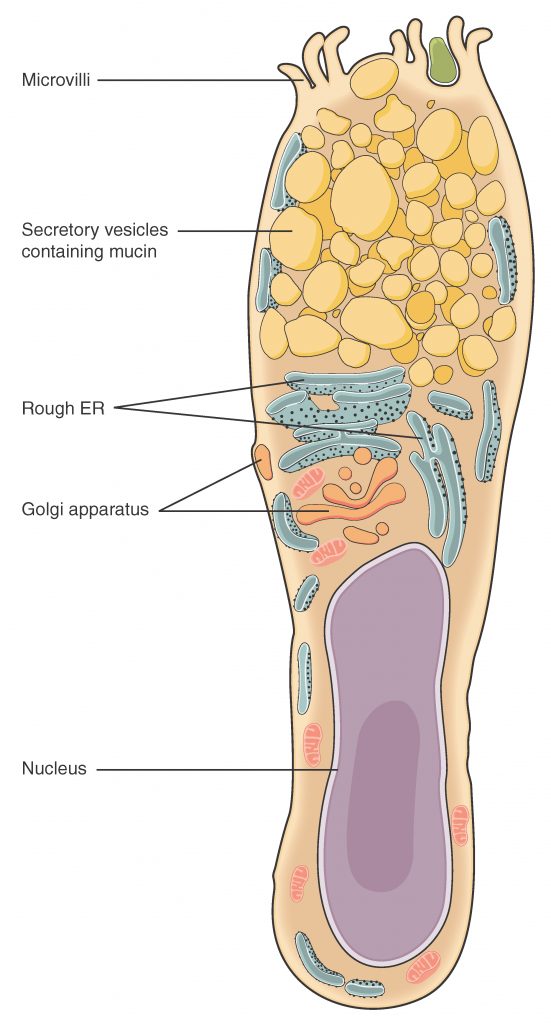
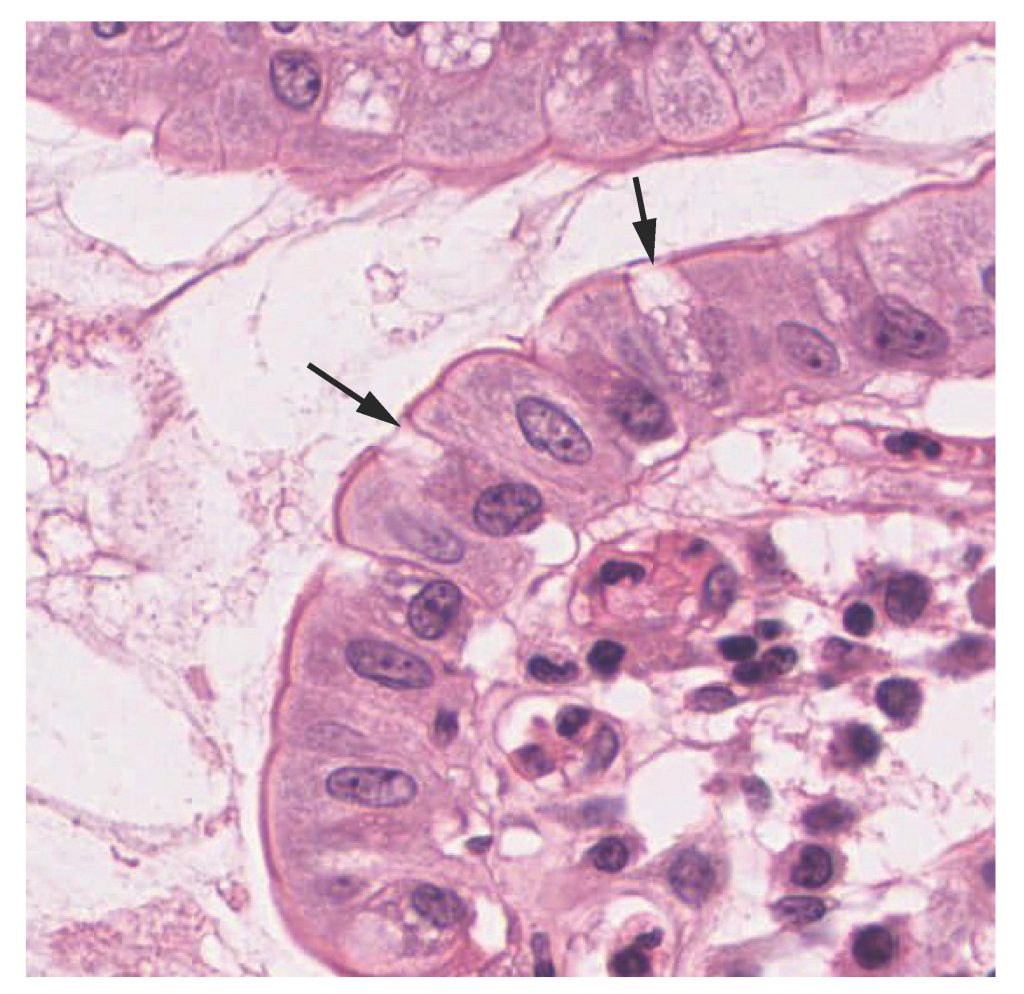
View the University of Michigan WebScope to explore the tissue sample in greater detail.
Stratified Epithelium
A stratified epithelium consists of several stacked layers of cells. This epithelium protects against physical and chemical wear and tear. The stratified epithelium is named by the shape of the most apical layer of cells, closest to the free space. Stratified squamous epithelium is the most common type of stratified epithelium in the human body. The apical cells are squamous, whereas the basal layer contains either columnar or cuboidal cells. The top layer may be covered with dead cells filled with keratin. Mammalian skin is an example of this dry, keratinized, stratified squamous epithelium. The lining of the mouth cavity is an example of an unkeratinized, stratified squamous epithelium. Stratified cuboidal epithelium and stratified columnar epithelium can also be found in certain glands and ducts, but are uncommon in the human body.
Another kind of stratified epithelium is transitional epithelium, so-called because of the gradual changes in the shapes of the apical cells as the bladder fills with urine. It is found only in the urinary system, specifically the ureters and urinary bladder. When the bladder is empty, this epithelium is convoluted and has cuboidal apical cells with convex, umbrella shaped, apical surfaces. As the bladder fills with urine, this epithelium loses its convolutions and the apical cells transition from cuboidal to squamous. It appears thicker and more multi-layered when the bladder is empty, and more stretched out and less stratified when the bladder is full and distended. The image below summarizes the different categories of epithelial cell tissue cells.

Glandular Epithelium
A gland is a structure made up of one or more cells modified to synthesize and secrete chemical substances. Most glands consist of groups of epithelial cells. A gland can be classified as an endocrine gland, a ductless gland that releases secretions directly into surrounding tissues and fluids (endo- = “inside”), or an exocrine gland whose secretions leave through a duct that opens directly, or indirectly, to the external environment (exo- = “outside”).
Endocrine Glands
The secretions of endocrine glands are called hormones. Hormones are released into the interstitial fluid, diffused into the bloodstream, and delivered to targets, in other words, cells that have receptors to bind the hormones. The endocrine system is part of a major regulatory system coordinating the regulation and integration of body responses. A few examples of endocrine glands include the anterior pituitary, thymus, adrenal cortex, and gonads.
Exocrine Glands
Exocrine glands release their contents through a duct that leads to the epithelial surface. Mucous, sweat, saliva, and breast milk are all examples of secretions from exocrine glands. They are all discharged through tubular ducts. Secretions into the lumen of the gastrointestinal tract, technically outside of the body, are of the exocrine category.
Glandular Structure
Exocrine glands are classified as either unicellular or multicellular. The unicellular glands are scattered single cells, such as goblet cells, found in the mucous membranes of the small and large intestine. The multicellular exocrine glands known as serous glands develop from simple epithelium to form a secretory surface that secretes directly into an inner cavity. These glands line the internal cavities of the abdomen and chest and release their secretions directly into the cavities.
Section Review
In epithelial tissue, cells are closely packed with little or no extracellular matrix except for the basal lamina that separates the epithelium from underlying tissue. The main functions of epithelia are protection from the environment, coverage, secretion and excretion, absorption, and filtration. Cells are bound together by tight junctions that form an impermeable barrier. They can also be connected by gap junctions, which allow free exchange of soluble molecules between cells, and anchoring junctions, which attach cell to cell or cell to matrix. The different types of epithelial tissues are characterized by their cellular shapes and arrangements: squamous, cuboidal, or columnar epithelia. Single cell layers form simple epithelia, whereas stacked cells form stratified epithelia. Very few capillaries penetrate these tissues.
Glands are secretory tissues and organs that are derived from epithelial tissues. Exocrine glands release their products through ducts. Endocrine glands secrete hormones directly into the interstitial fluid and blood stream.
Review Questions
1. Where in the body would one find non-keratinizing stratified squamous epithelium?
- The inside of the mouth, esophagus, vaginal canal, and anus
- Only on the skin on the sole of the foot
- Inside of the mouth only
- Alveolar walls in lungs
2. In observing epithelial cells under a microscope, the cells are arranged in a single layer and look tall and narrow, and the nucleus is located close to the basal side of the cell. The specimen is what type of epithelial tissue?
- Stratified
- Columnar
- Squamous
- Transitional
3. Which of the following is the epithelial tissue that lines the interior of blood vessels?
- Columnar
- Pseudostratified
- Simple squamous
- Transitional
4. Which type of epithelial tissue specializes in moving particles across its surface and is found in airways and lining of the oviduct?
- Transitional
- Stratified cilated columnar
- Pseudostratified ciliated columnar
- Stratified squamous
Answer Key
1. The inside of the mouth, esophagus, vaginal canal, and anus
2. Columnar
3. Simple squamous
4. Stratified ciliated columnar
Adaption
This chapter is adapted from the following text:
Epithelial Tissue in Anatomy and Physiology by OSCRiceUniversity is licensed under a Creative Commons Attribution 4.0 International License
Media Attributions
- Types of Cell Junctions © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- Epitheleal Tissue © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 404_Goblet_Cell_new © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 404b_Goblet_Cell_new © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 423_Table_04_02_Summary_of_Epithelial_Tissue_CellsN © OSCRiceUniversity is licensed under a CC BY (Attribution) license
Tissue that lines vessels of the lymphatic and cardiovascular system, made up of a simple squamous epithelium.
Point of cell-to-cell contact that connects one cell to another in a tissue.
The part of a cell or tissue which, in general, faces an open space.
A matrix containing collagen and elastin secreted by connective tissue; a component of the basement membrane.
In epithelial tissue, a thin layer of fibrous material that anchors the epithelial tissue to the underlying connective tissue; made up of the basal lamina and reticular lamina.
Mechanically attaches adjacent cells to each other or to the basement membrane.
Simple squamous epithelial tissue which covers the major body cavities and is the epithelial portion of serous membranes.
Tissue that consists of a single layer of flat scale-like cells; promotes diffusion and filtration across surface.
Tissue that consists of a single layer of cube-shaped cells; promotes secretion and absorption in ducts and tubules.
Tissue that consists of a single layer of column-like cells; promotes secretion and absorption in tissues and organs.
Tissue that consists of a single layer of irregularly shaped and sized cells that give the appearance of multiple layers; found in ducts of certain glands and the upper respiratory tract.
Unicellular gland found in columnar epithelium that secretes mucous.
Tissue that consists of two or more layers of cube-shaped cells, found in some ducts.
Tissue that consists of two or more layers of column-like cells, contains glands and is found in some ducts.
Form of stratified epithelium found in the urinary tract, characterized by an apical layer of cells that change shape in response to the presence of urine.
Groups of cells that release chemical signals into the intercellular fluid to be picked up and transported to their target organs by blood.
Group of epithelial cells that secrete substances through ducts that open to the skin or to internal body surfaces that lead to the exterior of the body.
A group of cells within the serous membrane that secrete a lubricating substance onto the surface.
Thin extracellular layer that lies underneath epithelial cells and separates them from other tissues.
Forms an impermeable barrier between cells.
Allows cytoplasmic communications to occur between cells.

