Acute Kidney Injury
Microscopic Anatomy of the Kidney
J. Gordon Betts; Kelly A. Young; James A. Wise; Eddie Johnson; Brandon Poe; Dean H. Kruse; Oksana Korol; Jody E. Johnson; Mark Womble; and Peter DeSaix
Learning Objectives
By the end of this section, you will be able to:
- Describe the structure of the filtration membrane.
- Identify the major structures and subdivisions of the renal corpuscles, renal tubules, and renal capillaries.
- Describe the histology of the proximal convoluted tubule, loop of Henle, distal convoluted tubule, and collecting ducts.
The renal structures that contribute to the function of the kidney cannot be seen by the naked eye. Therefore, microscopy is required to reveal these structures.
Nephrons: The Functional Unit
Nephrons take a simple filtrate of the blood and modify it into urine. The filtrate is altered through reabsorption of nutrients and secretion of waste products until urine is formed. The term “forming urine” will be used to describe the filtrate as it is modified into “true urine”. The main tasks of the nephrons is to regulate the composition of the blood to achieve homeostasis and to excrete waste products and potential toxins in the urine. They do this by accomplishing three primary functions—filtration, reabsorption, and secretion.
Renal Corpuscle
As discussed earlier, the renal corpuscle consists of a network of capillaries called the glomerulus that is surrounded by Bowman’s (glomerular) capsule. Bowman’s capsule surrounds the glomerulus to form a lumen, and captures and directs this filtrate to the proximal convoluted tubule (PCT). Podocytes are the cells that cover the glomerular capillaries by extending finger-like arms called pedicels over them. Between the pedicels there are specialized slits that allow for filtration of the blood. As blood passes through the glomerulus, 10 to 20 percent of the plasma filters between these sieve-like fingers to be captured by Bowman’s capsule and funneled to the PCT. The glomerular capillaries have fenestrations, or “windows” in their walls that allow the filtrate to exit the capillary and be filtered by the pedicels. The fenestrations prevent filtration of blood cells or large proteins, but allow the passage of most other blood components, like water, electrolytes, and small molecules.
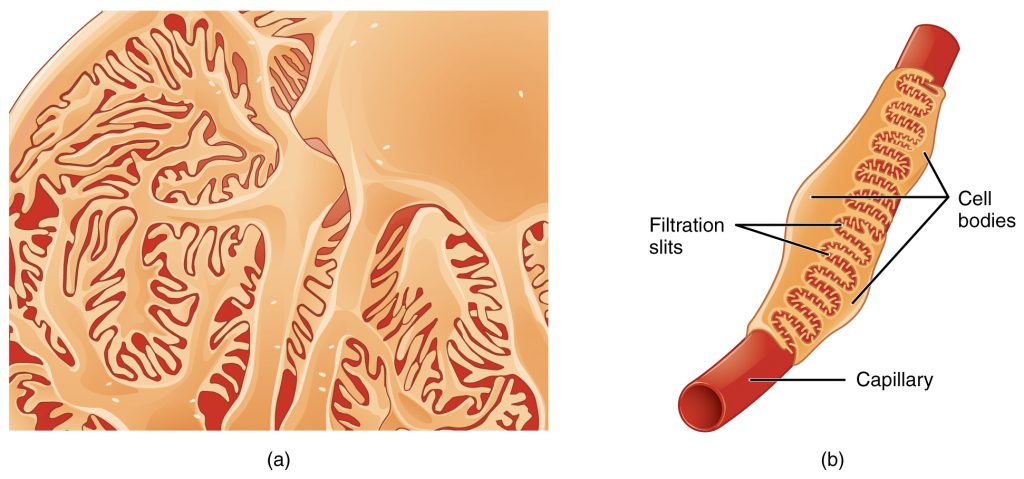
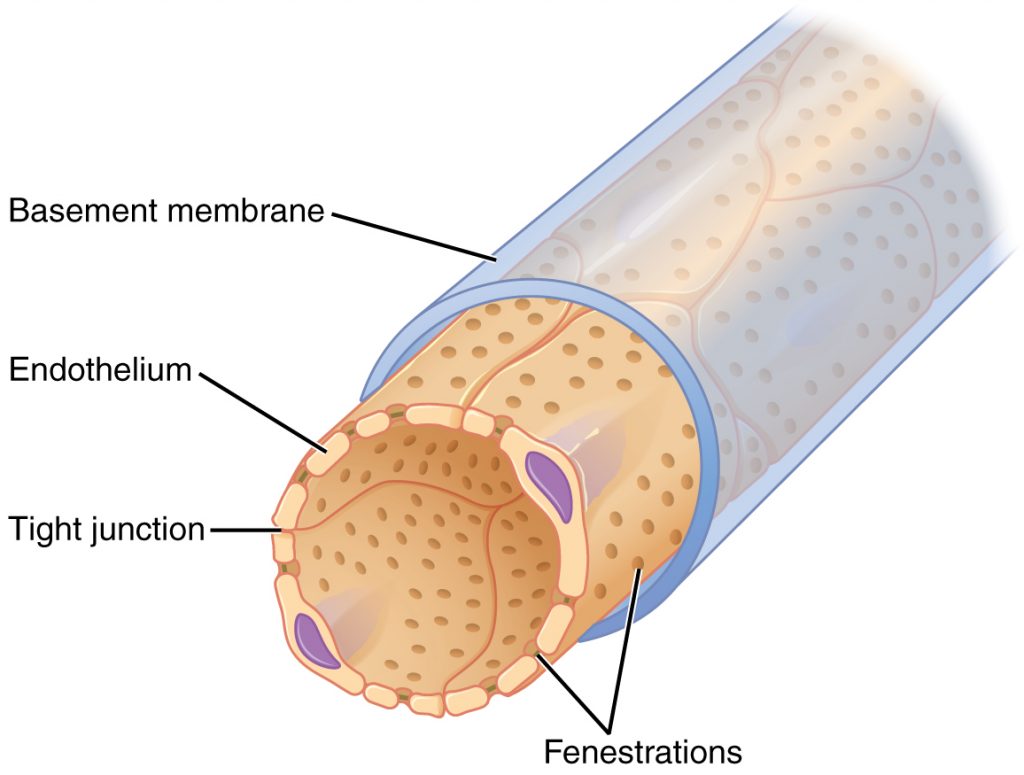
Proximal Convoluted Tubule (PCT)
Filtered fluid collected by Bowman’s capsule enters into the PCT. It is called convoluted due to its twisting path. A single layer of cells line the tubule and have folding of their cell membranes which creates microvilli, forming a brush border. These microvilli create a large surface area to maximize the absorption and secretion of solutes (Na+, Cl–, glucose, etc.), which is the main function of this portion of the nephron. These cells actively transport ions across their membranes, so they have many mitochondria to produce sufficient ATP.
Loop of Henle
The descending and ascending portions of the loop of Henle are continuations of the same tubule which descends into the deep cortex and medulla and returns to the cortex to form the distal convoluted tubule. Its function will be discussed in a subsequent section.
Distal Convoluted Tubule (DCT)
The DCT, like the PCT, is twisty, but it is shorter than the PCT. These cells are not as active as those in the PCT; thus, they have fewer microvilli. These cells also require ATP to pump ions against their concentration gradient, so you will find of large numbers of mitochondria, although fewer than in the PCT.
Collecting Ducts
The collecting ducts are continuous with the nephron but not technically part of it. In fact, each duct collects filtrate from several nephrons for final modification. Collecting ducts merge as they descend into the medulla and empty at papillae. In states when the body needs to keep more water, a hormone called antidiuretic hormone (ADH) signals the cells of the collecting ducts to produce protein channels called aquaporins, which selectively allow water to be reabsorbed instead of excreted in the urine.
Aquaporin Water Channel
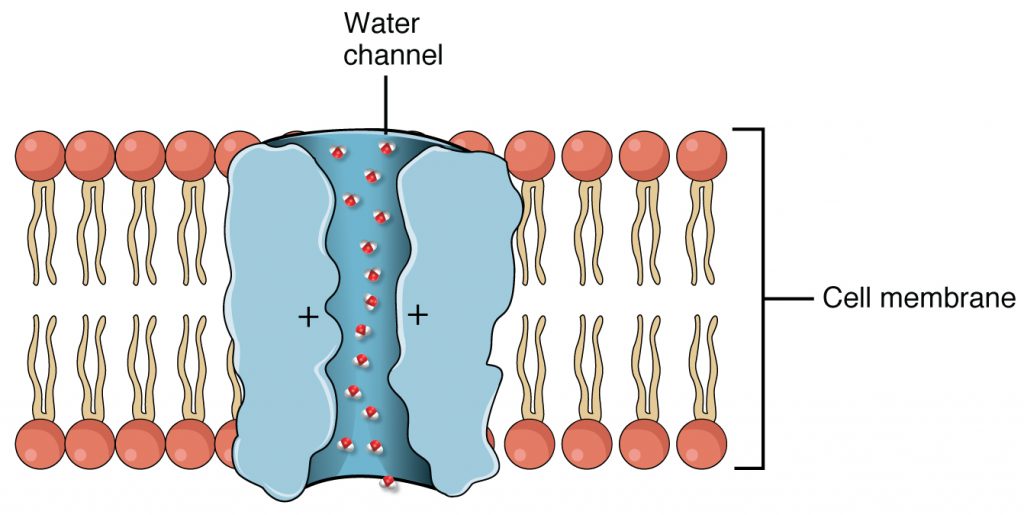
Section Review
The functional unit of the kidney, the nephron, consists of the renal corpuscle, PCT, loop of Henle, and DCT. The glomerulus is a capillary bed that filters blood principally based on particle size. The filtrate is captured by Bowman’s capsule and directed to the PCT. The filtrate enters the PCT where absorption and secretion of several substances occur. The loop of Henle descends into the medulla then returns to the cortex. Absorption and secretion continue in the DCT but to a lesser extent than in the PCT. Each collecting duct collects forming urine from several nephrons and responds to hormone signals by inserting aquaporin water channels into the cell membrane to fine tune water recovery.
Review Questions
1. Finish the following sentence. Blood filtrate is captured in the lumen of the:
- Glomerulus
- Bowman’s capsule
- Calyces
- Renal papillae
2. Finish the following sentence. The functional unit of the kidney is called the:
- Hilum
- Corpuscle
- Nephron
- Bowman’s capsule
Answer Key
- Bowman’s capsule
- Nephron
Adaption
This chapter is adapted from the following text:
Microscopic Anatomy of the Kidney in Anatomy and Physiology by OSCRiceUniversity is licensed under a Creative Commons Attribution 4.0 International License
Media Attributions
- 2613_Podocytes © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2614_Fenestrated_Capillary © OSCRiceUniversity is licensed under a CC BY (Attribution) license
- 2625_Aquaporin_Water_Channel © OSCRiceUniversity is licensed under a CC BY (Attribution) license
twisted tubules receiving filtrate from Bowman’s capsule; most active part of the nephron in reabsorption and secretion
descending and ascending portions between the proximal and distal convoluted tubules
portions of the nephron distal to the loop of Henle that receive hyposmotic filtrate from the loop of Henle and empty into collecting ducts

