Chapter 2. Patient Assessment
2.9 Head-to-Toe Assessment: Abdominal / Gastrointestinal Assessment
Checklist 19 provides a guide for subjective and objective data collection in an abdominal / gastrointestinal assessment.
Objective DataConsider the following observations:
|
|
Steps |
Additional information |
Overall Appearance: Observe for abdominal distension, stretch marks, contour, symmetry, presence and type of ostomy, overweight or underweight.
  |
Abdominal distension may indicate ascites associated with conditions such as heart failure, cirrhosis, cancer, and pancreatitis.
An abdomen that appears thin with little adipose tissue might suggest nutrition issues. It is important for the nurse to ask “is this normal for your abdomen” to help differentiate patient “norm” to signs and symptoms that may indicate an acute issue. Unusual findings may indicate compromised GI function.
|
| Auscultate Bowel Sounds
 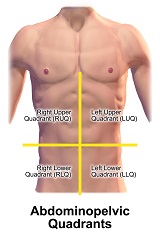 |
Divide the abdomen into quarters. Auscultate in each quadrant for evidence of gurgling, which suggests peristalsis.
Hyperactive bowel sounds may indicate bowel obstruction, gastroenteritis, or subsiding paralytic ileus. Hypoactive or absent bowel sounds may be present after GI surgery or when peritonitis or paralytic ileus are present. |
| Palpate Lightly in All Four Quadrants for Distension, Firmness, Masses, Pain | Firmness may indicate excess gas, ascites, peritonitis. Always ask the patient “is this normal for you?” |
| Observe stool to identify important characteristics. | Sometimes observing stool is an important part of the assessment process. Characteristics of bowel movements can assist with diagnosis and to help determine effectiveness of treatment for bowel related conditions.
Resource: Bladder and Bowel Foundation (nd). Bristol Stool Chart. https://www.bladderandbowel.org/wp-content/uploads/2017/05/BBC002_Bristol-Stool-Chart-Jan-2016.pdf |
Subjective Data |
|
| Focused GI assessment may also include ostomy assessment. See Chapter 11: Ostomy Care |
Potential GI related nursing diagnoses:
|
| Data sources: Assessment Skill Checklist, 2014; Jarvis, Browne, MacDonald-Jenkins, & Luctkar-Flude, 2014; Potter et al., 2019; Stephen, Skillen, Day, & Jensen, 2012; Wilson & Giddens, 2013 |
Critical Thinking Exercises
- A patient who experiences intermittent constipation asks what they might do to promote bowel regularity. Describe three nursing interventions that the nurse might discuss.
- Describe the character of stool expected from an ileostomy.
Attributions:
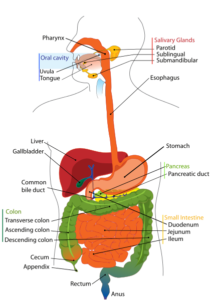
Figure 2.18 Gastrointestinal Tract by Mariana Ruiz, Jmarchn is in the public domain.
Figure 2.19 Big Man Big Stomach by Mike Baird is used under a CC BY 2.0 license.
Figure 2.20 Ileostomy with Bag by Remedios44 is used under a Creative Commons Attribution-Share Alike 4.0 International license.
Figure 2.21 Abdominopelvic Quadrants by Bruce Blaus is used under a Creative Commons Attribution 3.0 Unported license.