Private: Chapter 9. Blood Glucose Monitoring
9.2 Glucometer Use
People with diabetes require regular monitoring of their blood glucose to help them achieve as close to normal blood glucose levels as possible for as much of the time as possible. The benefits of maintaining a blood glucose level that is consistently within the range of 4 to 7 mmol/L will reduce the short-term, potentially life-threatening complications of hypoglycemia as well as the occurrence rate and severity of the long-term complications of hyperglycemia (Canadian Diabetes Association, 2018).
Patients in the acute care settings are likely to have inconsistent blood glucose levels, as they are affected by changes in diet and lifestyle, surgical procedures, the stress of being in a hospital and the stress of an acute illness. The prescriber will often prescribe the frequency of blood glucose monitoring, and sometimes this is left to the nurse’s discretion. In acute situations, a sliding-scale for insulin will be prescribed. The sliding scale provides direction for the type and dose of insulin in response to specific blood glucose readings.
At home, the frequency of blood glucose monitoring will depend on many factors including the type of diabetes, the type of antidiabetic medication, changes to medications, adequacy of glycemic control, literacy and numeracy skills, patterns of hypoglycemia, awareness and recognition of hypoglycemic symptoms, occupational requirements, and acute illness (Canadian Diabetes Association, 2018). The diabetes educator and/or prescriber may suggest frequency of blood glucose monitoring.
In hospital, it is usually the responsibility of the nurse to perform blood glucose readings. As with any clinical procedure, ensure that you understand the patient’s condition, the reason for the test, and the possible outcomes of the procedure. Prior to performing a blood glucose test, ensure that you have read and understood the manufacturer’s instructions and your agency’s policy for the blood glucose monitoring machines used in your clinical setting, as these vary. It is also important that you determine the patient’s understanding of the procedure and the purpose for monitoring blood glucose level. Before you begin, you should also determine if there are any conditions present that could affect the reading. For example, is the patient fasting? Has the patient just had a meal? Is the patient on any medications that could affect the reading? In these situations, draw on your knowledge and understanding of diabetes, the medication you are administering, the uniqueness of your patient, and the clinical context. Use your knowledge and critical thinking to make a clinical judgment.
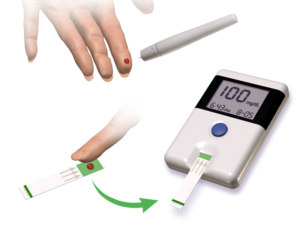
Inspect the area of skin that will be used as the puncture site, and ask the patient if they are in agreement with the site you have identified to use for the skin puncture. Your patient may have a preference for the puncture site. For example, some patients prefer not to use a specific finger for the skin puncture. Or a particular site may be contraindicated. For example, you shouldn’t use the hand on the same side as a mastectomy.
Patients who do their own blood glucose testing at home may prefer to handle the skin-puncturing device themselves and continue self-testing while they are in the hospital.
Checklist 79 outlines the steps for taking a skin-puncture blood sample and using a blood glucose monitor (glucometer) to measure a patient’s blood glucose level.
Checklist 79: Blood Glucose MonitoringDisclaimer: Always review and follow your agency policy regarding this specific skill. |
|||
Safety considerations:
|
|||
Steps |
Additional Information |
||
| 1. Review the patient’s medical history for diabetes type, medications, and/or anticoagulant therapy. | A thorough knowledge of the patient’s medical history is important even when the test performed is a relatively simple procedure.
Anticoagulant therapy may result in prolonged bleeding at the skin-puncture site and require pressure to the site. |
||
| 2. Determine if the test requires special timing; for example, before or after meals. Blood glucose monitoring is usually done prior to meals and the administration of antidiabetic medications. | Blood glucose levels are affected by diet, and the test may be scheduled at very specific intervals.
Diet and medication orders are based on the assumption that the test results are accurate. |
||
3. Gather equipment needed:
|
Having equipment prepared and available promotes organization, safety, and timeliness.
Check your agency guidelines about the use of alcohol or soap and warm water to clean puncture site prior to puncture. Alcohol use on the skin over time may cause the skin to dry out and become more fragile. 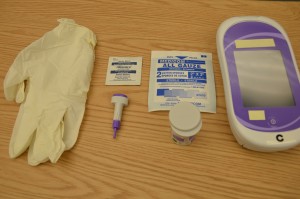 |
||
| 4. Determine if blood glucose meter needs to be calibrated. | Calibration / quality control checks should be done regularly according to agency policy to ensure accuracy of readings. | ||
| 5. Assess patient’s sites for skin puncture. | Skin that is intact at the puncture site minimizes the risk of infection and promotes healing.
Usually fingers are used for glucose testing. |
||
| 6. Perform hand hygiene. | Hand hygiene prevents the transfer of microorganisms. | ||
| 7. Have patient wash hands with soap and warm water, and position the patient comfortably in a semi-upright position in bed or upright in a chair. Encourage patient to keep hands warm.
Hospital policy may require use of an alcohol swab only, not water, to clean the puncture site. Ensure that puncture site is completely dry prior to skin puncture. |
Washing reduces transmission of microorganisms and increases blood flow to the puncture site.
  |
||
| 8. Remove a reagent strip from the container and reseal the container cap. Do not touch the test pad portion of the reagent strip. | Tight closure of the container keeps strips from damage due to environmental factors.
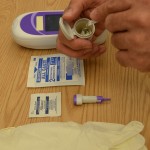 |
||
| 9. Follow the manufacturer’s instructions to prepare the meter for measurement. | This prepares meter for accurate readings.
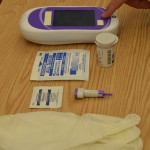 |
||
| 10. Place the unused reagent strip in the glucometer or on a clean, dry surface (e.g., paper towel) with the test pad facing up. This step is dependent on the manufacturer’s instructions. |
 Moisture may alter the test results. |
||
| 11. Apply non-sterile gloves. |
 Gloves protect health care provider from BBF exposure. |
||
| 12. Keep area to be punctured in a dependent position. Do not milk or massage finger site. | The finger in a dependent position will increase blood flow to the area. Milking or massaging the finger may introduce excess tissue fluid and hemolyze the specimen. | ||
| 13. Select appropriate puncture site and perform skin puncture. | Your patient may have a preference of site used. For example, the patient may prefer not to use a specific finger for the skin puncture. Avoid fingertip pads; use sides of finger.
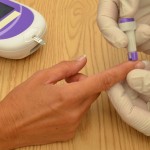 |
||
| 14. Gently squeeze above the site to produce a large droplet of blood. | Do not contaminate the site by touching it.
The droplet of blood needs to be large enough to cover the test pad on the reagent strip. 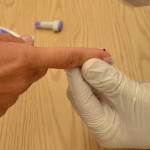 |
||
| 15. Transfer the first drop of blood (or second drop depending on the manufacturer’s instructions) to the reagent strip and apply following the manufacturer’s instructions. | The test pad must absorb the droplet of blood for accurate results. Smearing the blood will alter results.
 The timing and specific instructions for measurement will vary between blood glucose meters. Be sure to read the instructions carefully to ensure accurate readings. |
||
| 16. Immediately press the timer on the meter (unless it starts automatically with insertion of reagent strip). | Timing is critical to produce accurate results.
Always check the manufacturer’s instructions because the technique varies between meters. |
||
| 17. Apply pressure, or ask patient to apply pressure, to the puncture site using a 2 × 2 gauze pad or clean tissue. |
 This will stop the bleeding at the site. |
||
| 18. Read the results on the unit display. | Each meter has a specified time for the reading to occur.
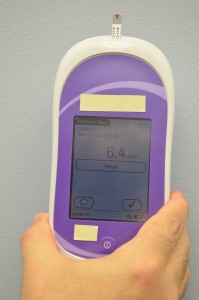 |
||
| 19. Turn off the meter and dispose of the test strip, 2 × 2 gauze, and lancet according to agency policy. | This reduces contamination by blood to other individuals. | ||
| 20. Remove non-sterile gloves and place them in the appropriate receptacle. | This reduces transmission of microorganisms.
 |
||
| 21. Perform hand hygiene. | This reduces the transmission of microorganisms. | ||
| 22. Review test results with the patient. | This promotes patient participation in health care. | ||
| 23. Document results according to agency policy. | Results will be used to determine the patient’s treatment plan. | ||
| Data source: Accu-Chek, n.d.; BCIT, 2015; Hortensius et al., 2011; Kaiser Permanente, n.d.; Pagana & Pagana, 2011; Perry et al., 2018; VCH & PHC Professional Practice, 2013; Weiss Behrend et al., 2004. | |||
Converting to Canadian (SI) Measurements
Many nursing resources are from the United States, where glucose values are reported as mg/dl. Canadian laboratories use the international system of units (SI), which are mmol/L. Therefore, you may need to convert your patient’s laboratory values to SI units. For glucose, divide the mg/dl by 18 to find the comparable SI unit (e.g., 65 mg/dl = 3.61 mmol/L). This conversion chart shows specific conversions.
Blood Glucose Readings that Require Follow-up
The concerns listed in Table 9.1 must be attended to and reported immediately to the relevant health care provider. Please consult hospital or unit-specific recommendations for exact values. The concerns and actions in Table 9.1 are guidelines only.
Table 9.1 Blood Glucose Readings that Require Follow-upAlways follow your agency’s protocols for excessively high or low blood glucose readings |
|
Concern |
Action |
| Blood sugar outside “acceptable range” (<2.2 mmol/L or >20 mmol/L) | Repeat capillary test to confirm. Initiate the agency’s hypoglycemic protocol if indicated. Report if reading remains out of range. Consider evaluation of blood glucose meter. |
| Blood sugar <2.2 mmol/L or >20 mmol/L | Order a stat blood glucose (venous sample) by laboratory staff . Initiate hypoglycemia if indicated. Consider evaluation of blood glucose meter. |
| Blood sugar <4 mmol/L | Initiate hypoglycemia protocol according to agency policy. |
| Preoperative blood sugar <4 mmol/L or >20 mmol/L | Initiate hypoglycemic protocol. Call prescriber. |
| Post-operative blood sugar >13.5 mmol/L (acceptable post-operative range = 8 to 13 mmol/L) | Notify prescriber. |
| Data source: BCIT, 2015; Canadian Diabetes Association, 2013; Perry et al., 2018 | |
Critical Thinking Exercises
- Describe two methods for increasing blood flow to a patient’s finger prior to lancing the finger.
- What is meant by sliding scale?
- If a patient is ordered insulin by sliding scale, when is the best time to check the glucose level?
Attributions
Figure 9.1. Glucometer by Bruce Blaus (2013) is used under a Creative Commons Attribution 3.0 Unported license.

