Chapter 8. Intravenous Therapy
8.11 Transfusion of Blood and Blood Products
All healthcare practitioners who administer blood or blood products must complete specific training for safe transfusion practices and be competent in the transfusion administration process. Always refer to your agency policy for guidelines for preparing, initiating, and monitoring blood and blood product transfusions. These guidelines apply to adult patients only.
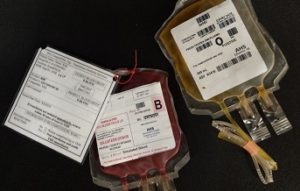
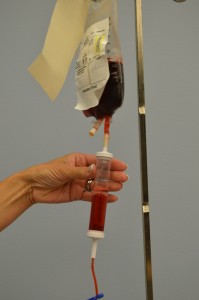
The transfusion of blood or blood products (see Figure 8.31) is the administration of whole blood, its components, or plasma-derived products. The primary indication for a red blood cell (RBC) transfusion is to improve the oxygen-carrying capacity of the blood (Canadian Blood Services, 2017a). An order from a healthcare provider is required for the transfusion of blood or blood products. RBC transfusions are indicated in patients with anemia who have evidence of impaired oxygen delivery. For example, individuals with acute blood loss, chronic anemia and cardiopulmonary compromise, or disease or medication effects associated with bone marrow suppression may be candidates for RBC transfusion. In patients with acute blood loss, volume replacement is often more critical than the composition of the replacing fluids (Canadian Blood Services, 2017a). Transfusions can restore blood volume, restore oxygen-carrying capacity of blood with red blood cells, and provide platelets and clotting factors. The most common type of blood transfusion is blood that is donated by another person (allogeneic). Autologous transfusion is the transfusion of one’s own blood (Perry et al., 2018).
Transfusion therapy is considered safe, and stringent precautions are followed in the collection, processing, and administration of blood and blood components. However, transfusions still carry risks such as incompatibility, human error, and disease transmission, and blood transfusion must be taken seriously at all times. Incompatibility can be decreased by using irradiated red blood cells or leukocyte-reduced blood. The majority of blood transfusion complications are a result of human error (Perry et al., 2018).
Compatibility testing is vital for all recipients of blood or blood products. Recipients must be transfused with an ABO group specific to their own blood type or ABO group-compatible. There are three types of blood typing systems: ABO, Rh, and human leukocyte antigen (HLA). For more information on these, refer to the online resources at the end of this chapter. It is vital to understand what types of blood groups are compatible for transfusions (Canadian Blood Services, 2017b).
When administering blood and blood products, it is important to know the patient’s values and beliefs regarding blood products. Some groups of individuals, mainly Jehovah’s Witnesses, may refuse blood transfusions or blood products based on religious beliefs. These individuals sometimes refuse transfusion of whole blood and primary blood components but may accept transfusion of derivatives of primary blood components such as albumin solutions, clotting factors, and immunoglobulins. Always assess each individual’s preference to establish if a blood component is an acceptable treatment to manage their illness or condition (Canadian Blood Services, 2017a).
When managing blood transfusions, it is important to identify issues promptly to manage reactions effectively. Transfusion reactions (mild to life-threatening) may occur despite all safety measures taken. All transfusion reactions and transfusion errors must be reported to the agency’s transfusion medical services (TMS, a.k.a. the “blood bank”). It is imperative to know what signs and symptoms to look for, and to educate your patient on what to report and when to report potential transfusion reactions. Mild to severe reactions may include the following (Canadian Blood Services, 2017b):
- Temperature ≥ 38.0°C or change of 1°C from pre-transfusion value
- Acute or delayed hemolytic transfusion reaction
- Hypotension/shock
- Rigors
- Anxiety
- Back or chest pain
- Nausea/vomiting
- Shortness of breath (dyspnea)
- Hemoglobinuria
- Bleeding/pain at IV site
- Tachycardia/arrhythmia
- Generalized flushing
- Rash ≥ 25% of body
- Urticaria and other anaphylaxis reactions
- Hemolysis after transfusion
- Cytopenias after transfusion
- Virus, parasite, and prion infections
- Non-immunological reactions including infection
- Circulatory overload
- Hypothermia
It is important to note that some reactions can occur one or more days after a transfusion (Canadian Blood Services, 2017b). As such, patients going home after a transfusion require education about what to watch for and what do do in the event of a reaction. For more information on types of reactions, signs and symptoms, and treatments, review the article adverse events related to blood transfusions, or see the online resources at the end of this chapter. If patient has a blood transfusion reaction, always follow agency policy to manage mild to severe blood reactions. This text will cover pre transfusion preparation (Checklist 75), transfusion of blood
and blood products (Checklist 76) and then managing a blood transfusion / blood product reaction (Checklist 77).
The steps in Checklist 75 must be completed before obtaining the blood or blood product from the blood bank (Alberta Health Services, 2015a, 2015b; Perry et al., 2018; Vancouver Coastal Health, 2008).
Checklist 75: Pre transfusion PreparationDisclaimer: Always review and follow your agency policy regarding this specific skill. |
||||
Safety considerations:
|
||||
Steps |
Additional Information |
|||
| 1. Verify prescribers’ order for the specific blood or blood product order | Order must verify the type of product; amount; date, time, rate or duration of the infusion; any modifications to the blood component; specific transfusion requirements; and sequence in which multiple components are to be transfused (if multiple components are ordered).
 |
|||
| 2. Verify the prescriber’s orders for any pre- or post-transfusion medications to be administered. | Medications given prior to transfusion are only considered for persons with documented moderate to severe reactions. Typically medications are administered 30 minutes prior to the transfusion. Examples of meds might include diphenhydramine, acetaminophen, and furosemide.
Remember: These medications can also mask a potential reaction. |
|||
| 3. Obtain the patient’s transfusion history, and note any known allergies and previous transfusion reactions. | Past complications may require patient to have pre- and post-transfusion medications to prevent further transfusion reactions. | |||
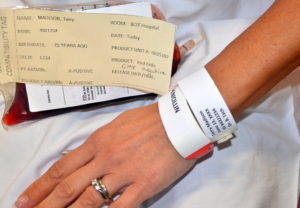
| 4. Check that the correct patient facility identification and TMS identification band are on the person.
If no facility identification band, apply one. If no TMS (a.k.a. blood band) present, STOP. Notify TMS. If any discrepancies STOP. Do not proceed until the discrepancy is resolved. |
Group, screen, and cross match must be completed within 96 hours of the transfusion to establish any new antibody formation and to ensure current compatibility.
If group and screen are outdated, initiate processes for new testing. Only TMS can apply blood product related bands. |
|||
| 5. Establish IV site or verify patency of current site. | IV sites must be patent and without complications.
Blood and blood products cannot be mixed with IV medications. If necessary, establish a site specifically for the blood product. The IV cannula must be large enough to allow flow of product at the correct rate. Generally for adults 20 to 22 gauge. Large cannulas are necessary for rapid infusion (i.e., 16 or larger). 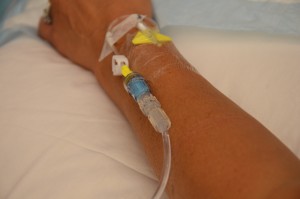 CVCs with multiple lumens may allow blood or blood products to be given simultaneously when medications and other solutions infuse through separate lumens. |
|||
| 6. Verify correct infusion equipment. Prime an IV line following Checklist 66.
Initiate primary IV @ 30 cc/hr. Ensure a back up line of 0.9% NS with a standard IV administration set is available at the bedside in the event of emergency. |
Blood components require filter tubing to remove clots, debris, and coagulated protein. A straight blood administration set is used for all transfusions (we no longer use Y’d blood tubing).
Glass bottles containing albumin and IVIG require vented tubing. If using a pressure infusion device, ensure it is safe to use with transfusions. Some infusion devices can cause mechanical hemolysis.
Refer to blood product fact sheets for all other products. If this is an elective transfusion, an alternate approach is to prime the IV administration set with the blood product just prior to administration. |
|||
| 7. Assess laboratory values to confirm rationale for transfusion. | For example Hgb, hematocrit, coagulation values, platelent count. This ensures the transfusion is appropriate. | |||
| 8. Check that the prescriber has obtained the necessary consent.
|
It is the prescriber’s responsibility to obtain consent for blood or blood products. | |||
| 9. The nurse confirms consent by ensuring the patient understands the procedure, rationale and by providing an opportunity for the patient’s concerns / questions to be answered.
RN to document confirmation of consent. |
Blood products require consent prior to administration.
Notify the prescriber if patient is unable to provide indication of understanding the proposed blood or blood product transfusions. |
|||
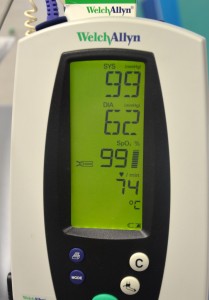
| 10. Obtain and record the pre-transfusion baseline vitals including temperature, pulse, respirations, blood pressure, and SpO2.
In addition, assess for other symptoms that may be confused with transfusion reaction. |
Fever, rashes, flank pain, or shortness of breath may be preexisting and thus difficult to differentiate from a transfusion reaction.
This assessment should be done within 30 minutes of initiating the transfusion. These serve as a baseline in which to compare any changes that may suggest transfusion reaction. |
|||
| 11. Have emergency equipment available at the bedside (oxygen, suction, etc.). | Be prepared for potential complications, as prompt intervention may be required to prevent serious complications.
 |
|||
| 12. Complete all documentation as required per agency policy.
|
Proper documentation provides evidence that all required procedures have been followed to prepare for a transfusion.
You have completed bedside check #1. You are now ready to call for the blood product. |
|||
| Data sources: Alberta Health Services, 2015b; Canadian Blood Services, 2017c; Interior Health, 2018; Perry et al., 2018; Vancouver Coastal Health, 2008 | ||||
| Data Sources: Alberta Health Services, 2015a, 2015b; Canadian Blood Services, 2017; Interior Health, 2018; |
Critical Thinking Exercises
- How long can blood or blood products be at room air temperature before being considered at risk for infusion?
- You are about to initiate an infusion of packed red blood cells. What patient teaching is important to include about possible signs and symptoms of reaction?
Attributions
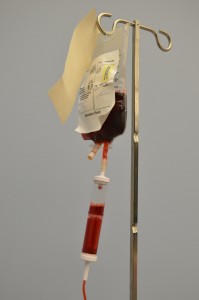
Figure 8.31. Red Blood Cells from BCIT is used under a CC BY-SA 4.0 international license.
Figure 8.32 Blood Product Example by author is licensed under a CC BY-SA 4.0 international license.