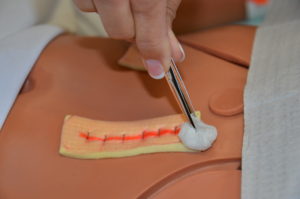
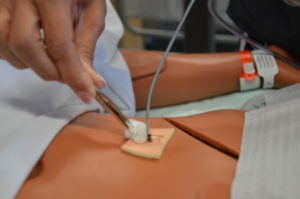
Chapter 4. Wound Care
4.5 Simple Dressing Change
The healthcare provider chooses the appropriate sterile technique and necessary supplies based on the clinical condition of the patient, the cause of the wound, the type of dressing procedure, the goal of care, and agency policy.
Agency policy will determine the type of wound cleansing solution, but sterile normal saline and sterile water are the solutions of choice for cleansing wounds and should be at room temperature to support wound healing. The ideal cleansing agent and the optimal method of wound cleansing has not been established conclusively (International Wound Infection Institute, 2016). Some wound cleansing solutions include sterile water, sterile saline, tap water, chlorhexidine, and povidone/iodine. Each cleansing solution has characteristics that make it a good or poor choice in certain situations. The nurse should use the wound cleansing solution as directed by agency policy and/or wound specialists.
Surgical dressings should remain in place for at least 48 hours and should be reinforced if soiled. At the 48 hour point, the wound may be exposed to air, but this is dependent on a number of factors such as type of surgery, wound healing (wound edges must be approximated and the wound not leaking), comfort of the client with an exposed incision, and agency policy (BC Provincial Skin and Wound Committee, 2011).
Checklist 35 outlines the steps for performing a simple dressing change.
Checklist 35: Simple Dressing ChangeDisclaimer: Always review and follow your agency policy regarding this specific skill. |
|||
Safety considerations:
|
|||
Steps |
Additional Information |
||
| 1. Assess current dressing. | If you plan to touch the dressing, donne non-sterile gloves to protect yourself from exposure to BBF. Assess dressing for signs of shadowing / bleeding, type and size of dressing used.
 |
||
| 2. Perform hand hygiene. | Hand hygiene reduces risk of spread of microorganisms.
 |
||
| 3. Gather necessary equipment. | Dressing supplies must be for single patient use only. Use the smallest size of dressing for the wound.
 Take only the dressing supplies needed for the dressing change to the bedside. Equipment that is contaminated at the bedside cannot return to general circulation to be used with other patients. |
||
| 4. Prepare environment; position patient; adjust height of bed; and turn on lights. | Ensure patient’s comfort prior to and during the procedure. Proper lighting allows for good visibility to assess wound. | ||
| 5. Perform hand hygiene. | Hand hygiene prevents spread of microorganisms.
 |
||
| 6. Prepare sterile field. |
 |
||
| 7. Add necessary sterile supplies. |
 |
||
| 8. Pour cleansing solution. |
 Normal saline or sterile water containers must be used for only one client, and they must be dated and discarded within at least 24 hours of being opened. |
||
| 9. Prepare patient and expose dressed wound. |
 |
||
| 10. Apply non-sterile gloves. | Use non-sterile gloves to protect yourself from contamination.
 |
||
| 11. Remove outer dressing with non-sterile gloves and discard as per agency policy. |
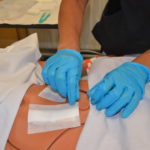 The rationale for non sterile gloves is to protect you from exposure to BBF. |
||
| 12. If necessary, remove inner dressing with transfer forceps. |
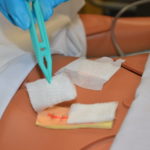 |
||
| 13. Discard transfer forceps & gloves |
  |
||
| 14. Assess wound | Are the wound edges approximated? Are the staples / sutures intact? Is there evidence of complications? | ||
| 14. Cleanse wound remembering principles of asepsis | Clean to dirty; one wipe one way discard; fluids flow in the direction of gravity.
|
||
| 15. Cleanse around the drain if present | Using a circular motion, clean the area immediately next to the drain and work outward still following principles of asepsis
|
||
| 16. Apply new sterile dressing. | The type of dressing applied will depend on the needs of the wound and the supplies available in the agency.
Secure dressings and drains with tape. Write the date and time on the outside of the dressing as a way to inform others. |
||
| 17. Ensure the patient is comfortable before leaving the bedside.
Perform hand hygiene.
|
Discard used equipment according to agency policy. | ||
| 18. Document according to agency policy.
Consider the progression of wound healing. If concerned notify the prescriber. |
Documentation example:
date / time: abdominal dressing changed. Moderate sanguinous drainage from distal end of incision. Wound well approximated. Staples intact. Cleansed with 0.9% NS. Dressed with medipore dressing. Patient tolerated well. ——- B. Dage RN
|
||
| Data source: BCIT, 2010a; Perry et al., 2018 | |||