Chapter 3. Safer Patient Handling, Positioning, Transfers and Ambulation
3.2 Body Mechanics
Body mechanics involve the coordinated effort of muscles, bones, and the nervous system to maintain balance, posture, and alignment during moving, transferring, and positioning patients. Proper body mechanics allows individuals to carry out activities without excessive use of energy, and it helps prevent injuries for patients and health care providers (Perry, Potter, & Ostendorf, 2018).
Musculoskeletal Injuries
A musculoskeletal injury (MSI) is an injury or disorder of the muscles, tendons, ligaments, joints or nerves, blood vessels, or related soft tissue including sprains, strains, or inflammation related to a work injury. MSIs are the most common health hazard for healthcare providers (WorkSafeBC, 2013). Table 3.1 lists risk factors that contribute to MSI.
Table 3.1 Factors that Contribute to MSIs |
|||
Factor |
Special Information |
||
| Ergonomic risk factors | Force: Lifting, lowering, carrying, pushing, pulling, and grip all involve force. Strong forces and light forces present risk for MSI.
Repetition: Refers to using the same group of muscles to complete a task over and over with little time for muscles to recover. Work posture: The position of different parts of the body, particularly awkward positions, can exert force on the muscles and bones, which causes strain. When a joint bends excessively or awkwardly, or outside its range of motion, MSI can occur. This also includes static postures. Workers need to change their body posture and move about periodically. Local contact stress: Refers to when hard or sharp objects come in contact with the skin, and the nerves and tissues become damaged by pressure. |
||
| Individual risk factors | Poor work practice; poor overall health (smoking, drinking alcohol, and obesity); poor rest and recovery; poor fitness, hydration, and nutrition | ||
| Data sources: Perry et al., 2018; WorkSafeBC, 2008; WorkSafeBC, 2013 | |||
When healthcare providers are exposed to ergonomic risk factors, they become fatigued and risk musculoskeletal imbalance. Additional exposure related to individual risk factors puts healthcare providers at increased risk for MSI (WorkSafeBC, 2013). Preventing MSIs is achieved by understanding the elements of body mechanics; applying the principles of body mechanics to all work-related activities; understanding how to assess a patient’s ability to position or transfer; and learning safe handling transfers and positioning techniques.
Elements of Body Mechanics
Body movement requires coordinated muscle activity and neurological integration. It involves the basic elements of body alignment (posture), balance, and coordinated movement. Body alignment and posture bring body parts into position to promote optimal balance and body function. When the body is well aligned, whether standing, sitting, or lying, the strain on the joints, muscles, tendons, and ligaments is minimized (WorkSafeBC, 2013).
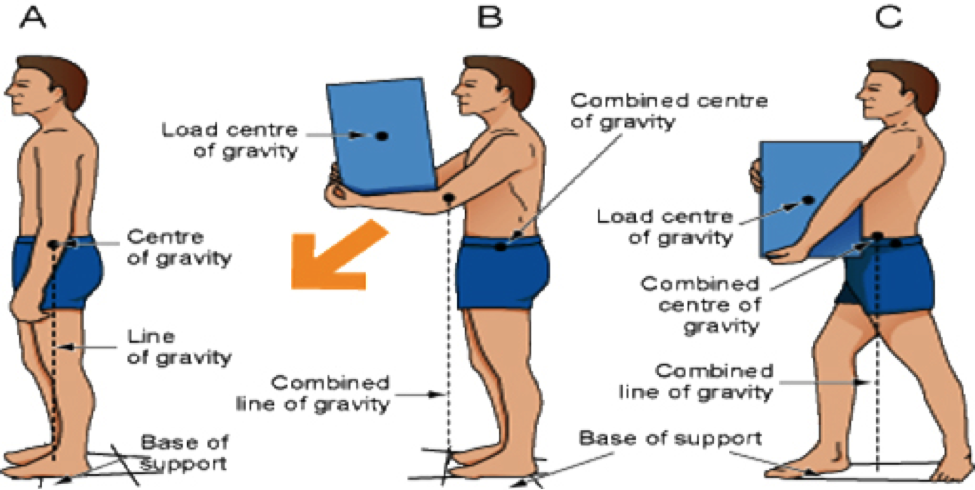
Body alignment is achieved by placing one body part in line with another body part in a vertical or horizontal line. Correct alignment contributes to body balance and decreases strain on muscle-skeletal structures. Without this balance, the risk of falls and injuries increases. In the language of body mechanics, the centre of gravity is the centre of the weight of an object or person. A lower centre of gravity increases stability. This can be achieved by bending the knees and bringing the centre of gravity closer to the base of support, keeping the back straight. A wide base of support is the foundation for stability and is achieved by placing feet a comfortable, shoulder-width distance apart. When a vertical line falls from the centre of gravity through the wide base of support, body balance is achieved. If the vertical line moves outside the base of support, the body will lose balance.
The diagram in Figure 3.1 demonstrates: (A) a well-aligned person whose balance is maintained and whose line of gravity falls within the base of support; (B) balance is not maintained when the line of gravity falls outside the base of support; and (C) balance is regained when the line of gravity falls within the base of support.
Principles of Body Mechanics
Table 3.2 describes the principles of body mechanics that should be applied during all patient-handling activities.
Critical Thinking Exercises
- How do body alignment and body balance contribute to proper body mechanics?
- John is asked to transfer a client from the bed to a stretcher. Name five principles of body mechanics John can implement to prevent a MSI.
Attributions
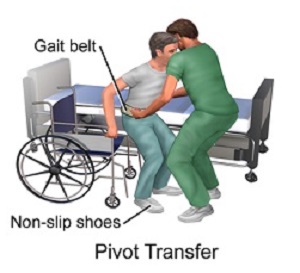
Figure 3.2 An illustration depicting how to transfer someone using the pivot method by BruceBlaus is used under a CC BY-SA 4.0 license.